
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Dressler's syndrome
Medical expert of the article
Last reviewed: 04.07.2025
Epidemiology
Previously, doctors believed that only 4% of patients suffered from Dressler syndrome after myocardial infarction. However, if we take into account all its low-symptom and atypical forms, we can say that it develops in 23% of cases. Some specialists even point to a higher prevalence rate – 30%. Over the past few years, the incidence of post-infarction syndrome has decreased. This can be explained by the widespread use of non-steroidal anti-inflammatory drugs and reperfusion therapy for infarctions by patients, which help reduce the level of myocardial damage.
Also, one of the reasons for the decrease in the number of patients with this disease can be called the use of various modern drugs that are part of complex therapy (statins, aldosterone antagonists, inhibitors of certain enzymes).
Causes Dressler syndrome
The main reason for the development of this syndrome is called necrosis or damage to cells in the muscle fibers of the heart, which occurs in patients after a heart attack. The decay products (myocardial and pericardial antigens) enter the blood, the patient develops autosensitization to proteins from destroyed cells, that is, autoimmune aggression develops.
Immune cells (cardiac reactive antibodies), which recognize foreign bodies, or so-called antigens, due to their identity in structure, begin to attack proteins that are located in the membrane structures of their own organs (lungs, heart, joints). That is, the body considers its own cells to be foreign and begins to fight them. The joint membranes become severely inflamed, but without the participation of pathogenic bacteria or viruses (the so-called aseptic inflammation). This causes quite severe pain.
Dressler syndrome occurs not only after transmural or large-focal infarctions, but also after cardiac surgeries. If the patient has a history of autoimmune diseases, the risk of complications increases.
Pathogenesis
In rare cases, this syndrome can develop after some traumatic injuries to the cardiac region (contusions, wounds, strong blow to the chest area).
Today, specialists consider Dressler syndrome as an autoimmune disease caused by pericardial and myocardial antigens and autosensitization. Great importance is also attached to the antigenic characteristics of the blood that has entered the pericardium. Patients with this syndrome have an elevated level of the C3d fraction. This can lead to complement-mediated tissue damage.
Patients also show some changes in cellular immunity. According to the latest data, the level of T-cells increases in Dressler syndrome.
Symptoms Dressler syndrome
The first symptoms may appear from two weeks to one month after the episode of myocardial infarction. The main signs of this disease are:
- The patient feels constant fatigue and weakness.
- The patient's body temperature rises (up to 39 degrees), which may decrease slightly between attacks.
- A common symptom of Dressler syndrome is pericarditis. There is a pressing and sharp pain in the chest area that may intensify during inhalation or coughing. The pain may radiate to the shoulder and neck.
- Pain in the lungs (pneumonitis), which may be accompanied by a dry cough, shortness of breath, and the appearance of blood when coughing.
- Painful sensations mainly on the left side of the chest (pleurisy), accompanied by a dry cough.
- Cardiobrachial syndrome – numbness in the left arm, a tingling sensation in the wrist area, marbled and too pale skin.
- Skin irritations – rashes that outwardly resemble allergic reactions.
- The collarbone and sternum area on the left side swells and may hurt.
Early Dressler syndrome
It develops within two weeks from the onset of myocardial infarction and is characterized by the development of dry pericarditis, which in 70% of cases is asymptomatic.
Only a small percentage of patients (15%) may experience dull and prolonged pain in the heart area after the first episode of myocardial infarction has been stopped, which has an increasing nature.
Where does it hurt?
Stages
There are several forms of Dressler syndrome:
- The extended or typical form is usually characterized by the following disorders: pleurisy, pericarditis, polyarthritis.
- Atypical form – characterized by the following symptoms: cardiobrachial syndrome, asthmatic and peritoneal syndrome, skin irritation, arthritis.
- Low-symptom or asymptomatic form – changes in blood composition, fever, arthralgia.
Complications and consequences
Patients with post-infarction syndrome may develop kidney pathologies, including autoimmune glomerulonephritis. Vessels may also be affected with the development of hemorrhagic vasculitis.
If not treated with hormonal drugs, the pericardial effusion may develop into adhesive pericarditis. This may lead to the development of restrictive heart failure.
Diagnostics Dressler syndrome
A cardiologist can make a diagnosis based on complaints received from patients with common symptoms that appear in the first two months after an episode of myocardial infarction. To confirm the diagnosis, an examination is performed - auscultation of the chest area in order to listen to possible noises from friction of the pericardium with the pleura. Moist rales in the lungs may also appear. To clarify the diagnosis, the following methods can also be used:
- Conducting a comprehensive blood test.
- Conducting an immunological study, biochemical blood analysis and rheumatological tests. In case of post-infarction syndrome, an increase in the level of C-reactive protein, troponin fraction and creatine phosphokinase will be observed.
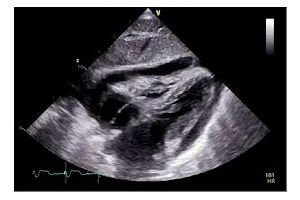
- Echocardiography – helps to identify thickening of the pericardium, fluid in the cavity and deterioration of its mobility.
- Performing a chest X-ray can diagnose pleurisy and pneumonitis.
- In some cases, an MRI of the thoracic region is prescribed.
 [ 27 ]
[ 27 ]
Tests
When conducting a blood test, the patient will notice the following changes:
- Leukocytosis.
- Often increased ESR.
- Eosinophilia.
- A sharp increase in C-reactive protein.
Dressler's syndrome must be differentiated from the following diseases:
- Recurrent or repeated myocardial infarction;
- Pneumonia of infectious etiology;
- pulmonary embolism;
- pericarditis and pleurisy.
What do need to examine?
How to examine?
Who to contact?
Treatment Dressler syndrome
For the treatment of Dressler syndrome, which has occurred for the first time, inpatient treatment is necessary. In case of relapses, outpatient treatment is possible if the patient's condition is not severe.
Non-steroidal anti-inflammatory drugs are most commonly used. If treatment with non-steroidal anti-inflammatory drugs has not yielded positive results, the cardiologist may recommend medium doses of some hormonal drugs. Anticoagulant treatment is not performed, but if there is a need to prescribe them, low doses are used.
Medicines
Glucocorticosteroid hormonal drugs:
- Dexamethasone is available as an injection solution. The active substance in the drug is dexamethasone sodium phosphate. It has antiallergic, anti-inflammatory, immunosuppressive effects. The dosage and duration of the course are prescribed by the attending physician. The drug is prohibited for use in patients with gastrointestinal diseases, viral and infectious diseases, immunodeficiency states, heart and vascular diseases, systemic osteoporosis, liver and kidney failure. Also, do not use to treat pregnant women. When treating with Dexamethasone, the following symptoms are possible: vomiting, hirsutism, steroid diabetes, headaches, euphoria, hallucinations, hypocalcemia, petechiae, allergies.
- Prednisolone is available in the form of tablets and injection solutions. The drug contains the active substance prednisolone sodium phosphate. It has antiallergic, anti-inflammatory and immunosuppressive effects. The dosage is determined in accordance with the patient's condition, so it is individual. Do not take patients with viral and infectious diseases, gastrointestinal diseases, immunodeficiency states, hypoalbuminemia. The drug is also prohibited during pregnancy. When taking, the following symptoms may appear: arrhythmia, vomiting, headaches, hirsutism, euphoria, disorientation, hypernatremia, acne, allergies.
Among nonsteroidal anti-inflammatory drugs, the most effective for the treatment of Dressler's syndrome are:
- Diclofenac - the drug contains the active ingredient diclofenac sodium. It has an analgesic, anti-inflammatory and antipyretic effect. Take one or two tablets once a day. The duration of the course is determined by the attending physician. Patients with gastrointestinal bleeding, gastrointestinal ulcers, hemophilia, intolerance to the components are prohibited from taking the drug. Do not use during pregnancy. When taking, the following are possible: abdominal pain, vomiting, headaches, tinnitus, dizziness, allergies, nephrotic syndrome.
- Indomethacin is a derivative of indoleacetic acid. It has analgesic, anti-inflammatory, and antipyretic effects. The dosage is determined by the attending physician individually. Do not take if you are intolerant to indomethacin, have pancreatitis, proctitis, chronic heart failure, arterial hypertension, or during pregnancy. The following symptoms may occur when taking it: nausea, headaches, tachycardia, anaphylactic reactions, allergies, mental disorders, and vaginal bleeding.
In some cases, acetylsalicylic acid is used:
- Aspirin - the drug contains the active substance acetylsalicylic acid. It has an antipyretic, analgesic, anti-inflammatory effect. The dosage is individual and prescribed by the attending physician. Patients with gastrointestinal ulcers, bronchial asthma, hemorrhagic diathesis, intolerance to the components are prohibited from taking the drug. Do not use during pregnancy. When taking the drug, the following are possible: allergic reactions, headaches, dizziness, vomiting, pain in the abdomen.
Forecast
With timely and correct treatment, the prognosis is favorable. It is worth understanding that patients with post-infarction syndrome need to lead a healthy lifestyle:
- Eat right, following the recommendations of nutritionists - eat fresh fruits and vegetables, juices, fruit drinks, cereals, replace animal fats with vegetable fats. Eliminate fatty meat, coffee, carbonated drinks, salty, fried, spicy and hot dishes from your diet. Eat as little salt as possible.
- Give up bad habits.
- Engage in moderate physical activity and exercise therapy (necessarily under the supervision of your doctor).
 [ 34 ]
[ 34 ]

