
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Cracks behind the ears in adults and children
Medical expert of the article
Last reviewed: 12.07.2025
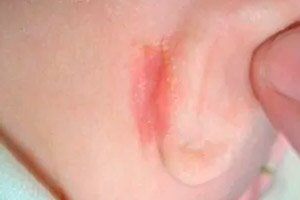
Dry or oozing skin and cracks behind the ears are considered by dermatologists as symptoms that indicate certain conditions or diseases that require identification for adequate treatment.
Causes ear cracks
Pointing out possible causes of cracking of the skin in the retroauricular – behind-the-ear region, experts name:
- irritating effects on the skin from hair care products and dyes, perfumes, earrings and ear piercings, eyeglass frames, hearing aids or headphones. In such cases, we are talking about allergic contact dermatitis; [ 3 ], [ 4 ]
- eczema or atopic dermatitis, which in pediatrics is most often called exudative diathesis; [ 5 ]
- fungal infections (dermatophytosis), which can affect skin folds of any location; [ 6 ]
- seborrheic dermatitis (known as dandruff); [ 7 ], [ 8 ]
- sebopsoriasis or seborrheic psoriasis of the scalp; [ 9 ]
- asteatic dermatitis (dyshidrotic or dry eczema, possible due to overdrying of the skin by frequent washing and insufficient general hydration, especially at low air humidity); [ 10 ], [ 11 ]
- spontaneous opening of the formed atheroma behind the ear. [ 12 ], [ 13 ]
The same factors cause cracks behind the ears in children. In addition, children with weakened immunity (as well as adults with severe immunosuppression) may experience scrofula or scrofulosis - an atypical mycobacterial infection caused by the saprophytic non-tuberculous bacterium Micabacterium scrofulaceum, [ 14 ] in severe cases causing inflammation of the cervical lymph nodes (usually in children in the first five years of life). [ 15 ]
Cracks behind the ears of a baby can be a consequence of diaper rash, which is common in children's skin folds at this age. Another common problem of babies with unregulated sebum production is the formation of gneiss or milk crusts on the head and behind the ears, which is essentially a manifestation of the same seborrheic dermatitis.
Risk factors
Risk factors for cracked skin behind the ears include:
- lack of vitamins A, E, B2, B6, E, D3;
- low zinc levels in the body;
- xerosis or dry skin (young children are more likely to have dry skin than adolescents); [ 16 ]
- disruption of the sebaceous glands of the skin;
- weakened immunity;
- genetic predisposition, childhood or old age;
- tendency to sensitization of the body or a history of allergies;
- infections.
Pathogenesis
Increased dryness of the skin is associated with large amounts of soap, which not only washes away dirt, but also removes protective sebum, without which moisture is not retained in the intercellular space of the epidermis, which leads to its cracking.
In addition, the acid mantle on the skin surface is destroyed - a natural barrier for bacteria and viruses. As is known, sebum is secreted by special glands and when mixed with the secretion of sweat glands, it forms an acid microfilm (skin pH from 4.5 to 6.2), which is called the mantle. At the same time, the normal pH of the blood is 7.4 (slightly alkaline), and this natural combination of different acidities of the external and internal environment is a non-specific factor in protecting the body from infections.
The pathogenesis of a chronic condition such as atopic dermatitis or eczema, which begins in early life, is quite complex and not fully understood; it is probably associated with a synergistic interaction of genetic factors, impaired barrier function of the epidermis and changes in its microbiome (bacterial colonization), as well as an increased immune response.
For example, genetics manifests itself in an abnormal decrease in the level of the secondary intracellular mediator cAMP (cyclic adenosine monophosphate), which controls cell activity, which leads to an increased release of histamine and leukotriene, which are involved in the immune response and are synthesized by mast cells and basophils.
And damage to the skin barrier in people with atopic dermatitis may be caused by mutations or deletions in the gene that codes for the skin protein filaggrin, which is involved in the formation of the stratum corneum.
In response to the destruction of the skin barrier, local inflammation develops through stimulation of Th2 cytokines (T-helper type 2), which produce interleukins.
See also - Atopic and allergic conditions
Seborrhea is associated with a fungal infection of the scalp called Malassezia furfur and often affects the skin along the hairline and the back of the ears, which may be diagnosed as seborrheic eczema.
Symptoms ear cracks
As in other areas of the body, atopic dermatitis around the ears causes symptoms such as dryness and desquamation (flaking) of the stratum corneum, redness, swelling of the subcutaneous tissue and itching, which may lead to painful cracks behind the ears.
With eczema, redness and cracking most often form at the point where the earlobe touches the skin.
When, with an eczematous reaction of the skin, weeping cracks form behind the ears, this means deeper damage to the skin with the seepage of exudate (formed from the intercellular fluid of damaged tissues).
With seborrheic dermatitis of the scalp, symptoms vary from slightly flaky skin (dandruff) to the formation of solid affected areas with redness and greasy horny scales. Moreover, such areas can be not only behind the ears, but also on the face (on the cheeks, on the eyebrows and eyelids, in the nasolabial folds). Some people experience swelling and flaking inside the auricles and auditory canals. [ 17 ]
Complications and consequences
When the integrity of the skin on the auricles is damaged, possible consequences and complications are associated with the addition of skin infections - bacterial or viral, as well as the aggravation of the course of dermatitis, which became the primary cause of the damage. [ 18 ]
For example, in atopic dermatitis, there is an alteration in the skin microbiome and a decrease in resistance against lipophobic pathogens, in particular Streptococcus pyogenes and Staphylococcus aureus bacteria (streptococci and staphylococci), which are often present on healthy skin. [ 19 ]
Penetrating into a crack in the skin, bacteria induce the production of immunoglobulins (Ig), which leads to the proliferation of T-lymphocytes and exacerbation of dermatitis.
Secondarily infected cracks behind the ears in an infant or young child can cause a long-term localized streptoderma that requires antibiotic treatment. [ 20 ]
With seborrhea and sebopsoriasis with severe itching leading to scratching of the skin, erythroderma may develop. [ 21 ], [ 22 ]
Diagnostics ear cracks
A crack behind the ear is visible to the naked eye, so a simple examination is often enough.
However, diagnostics in dermatology should reveal the true cause of this symptom. Therefore, blood tests may be required: general, sugar level, thyroid hormones, antibodies (Ig). And instrumental diagnostics includes dermatoscopy.
Differential diagnosis
Differential diagnosis is made based on the results of a more thorough and comprehensive dermatological examination of the skin.
Who to contact?
Treatment ear cracks
Treatment of cracked ears, in particular the choice of therapeutic agents, usually depends on the underlying cause of their occurrence.
Keeping the skin clean, dry and moisturized helps many people. Remedies for excessively dry skin and how to use them are presented in the material - Dry skin of the body.
After examination, the doctor prescribes medications, and these are, as a rule, external use products. If an inflammatory focus appears with eczema behind the ears, a combination of antibiotics and topical steroids will be needed, that is, ointments that relieve inflammation, primarily such effective products as Levomekol and Baneocin. [ 23 ]
What means are used, read in the publications:
- Treatment of diaper rash
- Treatment of atopic dermatitis
- Ointments for atopic dermatitis
- Eczema Creams
- Ointment for seborrheic dermatitis
To treat complications – streptococcal inflammation – ointments for streptoderma are used.
Homeopathy can also be used with ointments such as Zincum ricini, Calendula, Graphites, Ledum palustre, Hypericum perforatum.
Vitamins of the essential group and zinc and selenium preparations may also be prescribed.
Traditional treatment is not excluded, see – Treatment of diathesis with traditional remedies.
Immediately after bathing (before the skin dries completely), the skin on the ears should be lubricated with almond or sea buckthorn oil, aloe juice, concentrated aqueous solution of mumiyo or propolis. It is recommended to apply essential oils of tea tree, calendula, borage, jojoba, diluted with almond or refined sunflower oil (5-6 drops of essential oil per teaspoon) to the cracks.
Children with exudative diathesis and cracked skin behind the ears are quickly helped by herbal treatment: hygienic procedures using decoctions of chamomile flowers and medicinal calendula, succession grass or plantain leaves.
Prevention
It is hard to disagree that cleanliness is the key to health, but when choosing body and hair detergents, dermatologists advise paying attention to their composition and avoiding brightly colored gels and shampoos with a strong smell.
There are no special preventive measures for this case, so doctors simply urge everyone to eat right (including eating less sweets and fatty foods) and to maintain a healthy lifestyle.
Forecast
After treatment, cracks behind the ears heal, but the reasons for their appearance (dry skin, dermatitis) in most cases remain. Therefore, doctors do not guarantee that this problem will not arise in the future.

