
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Wart nevus
Medical expert of the article
Last reviewed: 12.07.2025
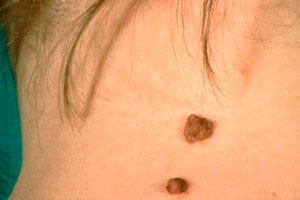
Among the benign pigmented formations on the skin – nevi (from the Latin naevus – birthmark) – a warty nevus protruding above the surface of the skin stands out, which, as the name suggests, resembles a wart.
In dermatology, due to this external similarity, such a mole is often defined as a warty nevus (from Latin verruca – wart) or as a papillomatous nevus, since the appearance of warts is provoked by the human papillomavirus (HPV). [ 1 ]
Epidemiology
Among all types of moles, the frequency of occurrence of warty nevi in the population does not exceed 6%. The prevalence of linear warty epidermal nevus is estimated at 1: 1000 live births. [ 2 ]
Causes wart nevus
The existence of several comparative definitions in medicine can be confusing for patients. But the warty epidermal nevus, which forms in the upper layer of the skin (epidermis), has nothing to do with warts (caused by viruses of the Papillomaviridae family). [ 3 ]
Like other types of moles on the body, a warty nevus in a child or adult
These nevi are the result of excessive growth (mitosis) of special dendritic cells of the basal layer of the epidermis and hair follicles - melanocytes, which contain and produce the dark pigment melanin, which provides photoprotection to skin cells.
More information in the materials:
Risk factors
In addition to heredity and intrauterine developmental characteristics, risk factors for the appearance of warty nevi include the negative impact of ultraviolet rays on epidermal cells, with prolonged exposure to which not only epidermal melanocytes, but also skin keratinocytes (the main cells of the outer layer of the dermis) can become more active. [ 4 ]
Pathogenesis
The pathogenesis of the development of wart-like epidermal nevi is chromosomal mosaicism, which can be caused by:
- mitotic recombination during embryogenesis of melanocytes from neural crest cells (melanoblasts);
- disruption of the movement of mature melanocytes to keratinocytes;
- changes in keratinocyte differentiation;
- mutations in genes encoding melanosome proteins (melanin synthesis) or melanogenic enzymes and hormones that regulate melanocyte proliferation and melanin synthesis. [ 5 ]
All details in the publications:
Symptoms wart nevus
The characteristic signs or symptoms of a warty nevus are the presence on the skin of a fairly convex, delimited formation of a dense structure (all shades of brown, dirty gray or bluish-violet tint), the surface of which is distinguished by the presence of tubercles. These irregularities are the result of alternating raised and slightly depressed areas of thickened epidermis with para or orthohyperkeratosis, that is, an increased level of keratin in nucleated and non-nucleated epithelial cells. [ 6 ]
Such a nevus may have a wide base (pedicle), which further resembles a wart. Another sign may be hair on a warty nevus.
When several areas of excessive melanocyte proliferation form, merging to form an extensive elongated thickening and hyperkeratosis of the epidermis, a linear warty nevus is diagnosed.
It should be borne in mind that nevi of a warty nature are not associated with inflammatory processes, however, extremely rarely in infancy or early childhood (and even more rarely in adults) an inflammatory linear warty nevus is possible. It is defined by dermatologists as a separate form of nevus with a characteristic unilateral localization (more often on the left - on the skin of the extremities) and a histological appearance: with thickening of the epidermis in the form of plaques and thickening of its spinous layer (acanthosis), as well as the presence of inflammatory infiltrates in the stratum corneum of the epidermis (which can have a spongy appearance). [ 7 ]
Complications and consequences
Possible complications and consequences are associated with damage to the nevus, which can result in bleeding and inflammation.
But a change in its color, shape, or a sharp increase in size is a serious reason to visit a dermatologist.
What is dangerous about a warty nevus? This is a benign neoplasm and, in principle, does not pose a danger, since it does not transform into melanoma. [ 8 ], [ 9 ]
Over time, the mole can increase in size, and an advanced warty nevus can be of significant size.
In some cases, a warty nevus itches, for more details see – Why does a mole itch and what to do?
Diagnostics wart nevus
Diagnosis of moles requires skin examination. Also required is a biopsy of the nevus (puncture or excisional, i.e. when it is removed) and histological analysis of the tissue.
As a rule, instrumental diagnostics is limited to dermatoscopy. [ 10 ]
Differential diagnosis
And differential diagnostics is carried out with skin papilloma and other epidermal formations. In particular, warty nevus or keratoma (either senile or follicular - focal keratinization of the epidermis in the area of the hair follicles) are differentiated, as well as dysplastic nevus, cystic epithelioma, Darier-Ferrand tumor, verruciform acrokeratosis, pigmented melanoma. [ 11 ]
Who to contact?
Prevention
There are no special preventive measures against the appearance of moles on the body.
Forecast
In the presence of a warty nevus, which is a benign formation, the prognosis is favorable.

