
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Why do vascular asterisks appear?
Medical expert of the article
Last reviewed: 06.07.2025
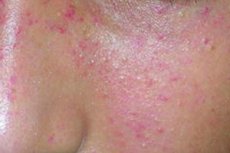
Stars are beautiful when you look at them in the sky or on the branches of a Christmas tree. On the human body, such “decorations” in the form of intertwined swollen capillaries called “vascular stars” do not look so attractive. In addition, they can appear in the most inconvenient places, for example, on the face or décolleté, on the nose or cheeks, arms, legs and other parts of the body. But some areas cannot be covered with clothing to hide the defect underneath. So you get such an indicator of ill health in the literal sense of the word, although it is not always about ill health that we are talking.
What are spider veins called?
If you think about it, spider veins are not quite the right name for a disease, which is a pathological dilation of capillaries associated with a violation of blood microcirculation. In addition, such formations of small vessels can have different shapes and be similar to snowflakes, spiders, a lattice, or represent separate slightly convex red, burgundy and even bluish stripes.
Vascular stars or nets are what people call these peculiar unwanted "decorations" on the body. In medical circles, the pathology is treated somewhat differently, so the scientific name of the phenomenon does not sound so pleasant - telangiectasia.
It is no coincidence that vascular neoplasms received this name. The term comes from 3 Greek words. The first part of the word, which we read as "tele", is derived from "telos", which in Russian means the ending. The second part, "angi", is transformed from "angeon" and means a vessel, a capillary, and the third - "ectasia" is an almost exact copy of the Greek word "ectasis", which means expansion, an expanded part. [ 1 ]
Depending on the shape of the capillary neoplasm, it can be called stellate or spider telangiectasia. If the tubercle of vessels has a bright red or burgundy color and its inner part noticeably protrudes above the surface of the skin like a mole, such vascular asterisks are often called angiomas (sometimes hemangiomas) due to the external similarity of pathologies.
The word "angioma" is usually used to denote a tumor consisting mainly of vessels (blood, lymphatic), which does not quite correctly reflect the essence of telangiectasias. After all, angioma is not a malignant proliferation of blood (or lymphatic) vessels, but telangiectasias are dilation of blood capillaries.
Spider veins in the form of single swollen capillaries in the facial area are called couperose in cosmetology. In dermatology, this same microcirculation disorder in small blood vessels is usually referred to as telangiectasias. [ 2 ]
Are spider veins dangerous?
Any new growths on the human body cause increased interest and some concerns. The worries are especially strong in this regard in our time, when information about the spread of oncological diseases, and skin cancer in particular, is pouring in from all sides.
We can reassure our readers that spider veins have nothing to do with malignant tumors. Just like angiomas, benign vascular tumors with a low probability of degenerating into cancer. Moreover, telangiectasias can be more likely to be considered a disorder than a disease, although they are often considered symptoms of certain liver pathologies, the cardiovascular system, or hereditary weakness of the connective tissue from which both capillary membranes are formed, and the proximity of the vessels to the skin surface (sometimes called thin skin).
In most cases, spider veins are considered more of a cosmetic defect that distorts the aesthetic appearance of a person’s body, especially if telangiectasias are located on exposed parts of the body and on the face. They can suddenly appear and disappear after some time, when the effect of the factor that caused them subsides. [ 3 ]
It should be said that the expansion of the lumen of venules, arterioles and capillaries, which are small vessels, does not pose a particular danger. Even if a neoplasm is accidentally damaged, there is no reason to be afraid of severe bleeding, because the speed of blood flow in capillaries is lower than in other, larger vessels. Another thing is that the wound can become a source of infection, which can spread throughout the body with the blood flow.
Telangiectasias may cause a feeling of aesthetic discomfort, but in general they are harmless. Much more dangerous are the underlying diseases that can cause spider veins to appear. Therefore, they should be considered as a signal to pay attention to your health. Checking your heart, liver and other vital organs, hormonal levels will not be superfluous. [ 4 ]
Cause
Spider veins can form from both small venous and arterial vessels (arterioles), not to mention capillaries, the walls of which are extremely thin and can stretch noticeably at high blood pressure. At the same time, telangiectasias should not always be considered a symptom of a disease. In a narrow sense, vascular networks and nodules act as a symptom of varicosis, liver cirrhosis, hepatitis. But in a broad sense, they can be considered a reflection of some syndrome or phenomenon, a reflection of processes occurring in the body.
Hereditary predisposition is one of the most important factors that determine the appearance of spider veins in some people and their absence in others who are in the same conditions. It is believed that solar radiation contributes to the appearance of vascular elements on the surface of the epidermis. But at the same time, some people do not hide from the sun and do not have such defects on their skin, while in others, spider veins immediately appear on exposed parts of the body.
The glycoprotein endoglin is a regulator of angiogenesis, i.e. the process of formation and development of vascular walls. Its deficiency, caused at the gene level, is transmitted to children in a dominant manner, i.e. the probability of a tendency to develop vascular pathologies (we are talking about a hereditary disease called hemorrhagic telangiectasia) is higher than the chance that the predisposition can be avoided. However, a high risk is said to exist if the dominant gene is transmitted from both parents.
Hemorrhagic telangiectasia is manifested by the formation of multiple vascular elements on the body and their bleeding.
A gene that causes high levels of the growth factor of the inner lining of blood vessels (endothelium) can also be inherited, which also leads to the appearance of spider veins.
Vascular wall weakness may be observed in congenital metabolic and autoimmune disorders. Thus, Raynaud's syndrome is characterized by vascular spasm, and in congenital connective tissue weakness syndrome, the vascular lining does not have the necessary elasticity and they expand under blood pressure. In this case, the expansion is persistent and irreversible, so the spider veins and small vessel networks that appear on the body do not disappear, as happens with hormonal imbalance. [ 5 ]
We have already said that telangiectasias, which form in the upper layers of the skin and consist of small diameter vessels (up to 1 mm), in the female body reflect the state of the hormonal background. Particular attention should be paid to estrogen.
In addition to the fact that this beneficial hormone prevents the formation of cholesterol plaques on the walls of blood vessels, it also dilates blood vessels, and multiple small capillaries located close to the epidermis become more visible. It is not surprising that pregnancy, when the level of this hormone increases, is one of the main risk factors for women of reproductive age. A decrease in estrogen levels in later stages of pregnancy is often accompanied by the disappearance of telangiectasias. But in some mothers, they disappear after childbirth, after several months.
But pregnancy is a temporary phenomenon, unlike menopause, when spider veins can also appear. And their appearance should not always be explained by venous congestion or hemodynamic disorders. Hormonal imbalance has a negative effect on almost all organs and systems. Surprisingly, a sharp decrease in estrogen levels also does not have the best effect on the condition of the vascular membranes. In this case, vascular changes will be more persistent than during pregnancy.
Risk factors for the appearance of spider veins also include abortions, miscarriages, and some gynecological pathologies (for example, ovarian cysts) that can affect hormonal levels. This also includes the use of hormonal contraceptive methods.
Since estrogen, which is much more abundant in the female body than in the male body, has a vasodilating effect on blood vessels, it turns out that spider veins appear more often in women than in men. This is confirmed by statistics. Men encounter such "decorations" 4 times less often than women, which is understandable (women have more reasons for vascular disorders).
Not only sex hormones have a dilating effect on blood vessels. Histamine, serotonin, and other vasoactive substances have the same property. If they are present in the body in increased quantities, the risk of spider veins becomes significantly higher. Anoxia (oxygen metabolism disorder), infections, and some physical effects against the background of hormonal changes or predisposition can be considered as triggers that start the pathological process in small vessels.
It should be said that spider veins are not only a "privilege" of adults. They can also appear in childhood. The cause may be hereditary predisposition and prolonged exposure to the sun, as well as skin injuries. Damage to the epidermis and deeper layers of the skin is often accompanied by damage to small vessels located in these areas (compression, rupture of the membrane). It is at the site of such damage that vascular elements in the form of convex stars, branches, nets, linear telangiectasias can form. Usually they do not last long and soon disappear, leaving no trace.
As we can see, spider veins can be considered both as a symptom of serious disorders in the body and as a reflection of physiological processes occurring in it. If you ignore them, you can miss a dangerous disease. But only a specialist can determine what the appearance of telangiectasias is associated with after a preliminary examination of the patient.
Pathogenesis
Spider veins can appear on different parts of the body. Their appearance on the legs is most explainable, and then such vascular defects are associated with a disease called "varicose veins" or simply "varicose veins". It is more difficult to understand the occurrence of vascular neoplasms in the face, neck, chest, upper limbs, etc.
It should be said that in some situations, the appearance of telangiectasias remains a mystery even for doctors who cannot establish the causes of the appearance of spider veins. This happens if all known options have been tried, but none of them are suitable for a specific situation.
But what actually causes spider veins? What pathological factors do doctors consider as possible causes of this phenomenon?
The following pathologies can be considered probable causes of the appearance of spider veins on the body:
- Cardiovascular diseases and, in particular, chronic vascular diseases. Most often in such cases, vascular nodules appear on the lower extremities in the area of the shins and thighs. It is important to understand that spider veins are not, in essence, specific symptoms of varicose veins, although a mild form of varicose veins (reticular varicose veins) does have certain similarities with telangiectasias (the appearance of foci of dilated small veins under the skin). This is a separate disorder, which in some cases can be considered a mild version of chronic vascular disease, and in others as a temporary phenomenon.
The common cause of varicose veins and telangiectasias is hereditary weakness of small vessels, metabolic and hormonal disorders (predisposing factors), [ 6 ], but varicose veins in most cases are caused by venous congestion (hemodynamic disorders) due to large body weight, regular compression of leg vessels, heavy loads while standing or sitting, wearing high-heeled shoes. Telangiectasias do not have such a relationship, and spider veins can also appear on other parts of the body. In this case, not only small veins are subject to expansion, but also arterioles carrying arterial blood, as well as capillaries, where gas exchange occurs (interchange of venous, oxygen-poor, and capillary blood), while the peculiar spider veins on the legs with varicose veins are seals from venous vessels that have lost their elasticity. [ 7 ]
Quite often, both varicose veins and telangiectasia (spider veins, neoplasms from small arteries) can be seen on the lower extremities. However, the appearance of spider veins is usually not accompanied by other symptoms of ill health (in some cases, patients may complain of pain and itching in the area of the neoplasm). Varicose veins, especially in the lower extremities, are also characterized by swelling of the legs, a feeling of heaviness in them at the end of the day, dull pain, and sometimes night spasms (cramps). [ 8 ]
A severe form of CVD is chronic venous insufficiency, which results in the appearance of numerous vascular networks of small and larger veins on the legs of patients (this cause is more typical for men).
- Liver diseases. It is not for nothing that the liver is considered one of the main filters of the body (along with the kidneys). This important organ helps remove poisons and toxins from the body, as well as dangerous substances formed during the life of the body itself. If the liver is sick, harmful substances accumulate in the body, causing various disorders.
Intoxication of the body affects the metabolic processes occurring in it. The body tries to remove all the "garbage" through the skin, which immediately becomes noticeable by the change in its appearance, the appearance of inflammatory elements, and local changes in pigmentation. Vessels (primarily small ones, which have a thin shell) lose their elasticity and can stretch and even burst under the pressure of blood.
The appearance of spider veins on the skin, which often occurs with liver cirrhosis, is also associated with organ dysfunction. Quite often, intoxication is the reason that the working tissue of the liver (parenchyma) changes its structure, degenerates into denser fibrous tissue, which cannot serve as a filter. Other causes of cirrhosis can be congestive heart failure, diseases of the biliary system, hereditary metabolic disorders, infections. But regardless of the cause of the disease, a decrease in the functionality of the organ is always noted.
Another serious liver disease is hepatitis. The disease can have different pathogens of infectious (viral) nature and transmission routes, therefore, hepatitis A, B and C are distinguished. However, the clinical picture of any of the hepatitis is reduced to the development of inflammation in the liver and a decrease in its functionality, as evidenced by yellowing of the skin, sclera, changes in the color of urine and feces, deterioration of the skin and small vessels. [ 9 ]
As with liver cirrhosis, spider veins with hepatitis appear primarily on the back and face (an inflammatory rash also often appears here), while with varicose veins, changes in the vessels often affect the surface of the lower extremities (less often the pelvic area, perineum, scrotum in men, etc.).
It is important to understand that venous insufficiency can also be caused by chronic liver diseases, and in this case, nodules and networks of dilated veins can appear in different parts of the body, including internal organs.
Spider veins and liver disease are related to each other as a pathology and its consequences. Whatever the name of the disease, but if the liver's performance is impaired, the body begins to be "decorated" with capillary networks, trees, spots. [ 10 ]
- Hormonal disorders (the most common cause of telangiectasia in women). They can be both pathological and physiological (pregnancy, menopause). The leading role in the appearance of spider veins is played by the female hormone estrogen. Its increased production increases the risk of vasodilation.
Often, patients complaining of vascular defects can also notice other skin changes, even with a healthy liver. We are talking about cellulite. Vascular spiders and cellulite are frequent neighbors, because they have similar roots. Vascular (venous) spiders are often considered a result of venous congestion. But the violation of the outflow of venous blood and stagnation of lymph in turn increase the permeability of blood vessels. The liquid part of the blood (plasma) seeps through the weakened vascular networks and accumulates in soft tissues, forming a peculiar pattern on their surface. The surface of the body becomes uneven, bumpy, similar in structure to the skin of an orange or tangerine. This explains the frequent proximity of vascular spiders and "orange peel".

