
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Myliar tuberculosis
Medical expert of the article
Last reviewed: 04.07.2025
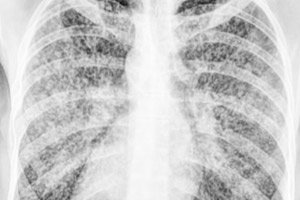
When the diffuse spread of tuberculosis bacteria in the body is accompanied by the appearance of many very small foci in the form of tubercles - tubercles or granulomas - nodules the size of a grain of millet (in Latin - milium), miliary tuberculosis is diagnosed).
Such tuberculosis foci in this type of disease can be found not only in the lungs, but also in other organs. [ 1 ]
Epidemiology
According to WHO data for 2018, tuberculosis was diagnosed in almost 10 million people, and about 1.6 million patients died from it. At the same time, experts say that on a global scale, about a third of the population may have a latent infection (especially in developing countries). [ 2 ]
Miliary pulmonary tuberculosis accounts for 1-2% of all cases of tuberculosis in this localization. And its extrapulmonary forms make up at least 20% of the total tuberculosis statistics. [ 3 ]
Causes miliary tuberculosis
As is known, the causes of tuberculosis are infection with Mycobacterium tuberculosis bacteria. The same pathogenic microorganism of the actinomycetes genus, which enters the body by airborne droplets, also causes multiple small-focal or disseminated miliary tuberculosis.
This progressive disease can occur during primary hematogenous or lymphogenous dissemination (spread) of mycobacteria throughout the body or affect other organs if existing tuberculosis is not treated.
See also - Disseminated pulmonary tuberculosis.
Is miliary tuberculosis contagious or not? Regarding the contagiousness of this type of infection with tuberculosis bacilli, there is an opinion that the degree of its contagiousness for others is lower, since it spreads through the blood (or lymph) flow.
Tuberculosis bacteria are transmitted from sick people, and tuberculosis is contagious when there are clinical symptoms indicating the activity of the pathogen. But if the mycobacterium does not lead to the development of the disease, that is, the infection in a person is latent (asymptomatic), he cannot infect others.
At the same time, as clinical experience shows, the result of the tuberculin skin test – the Mantoux test – is often false negative, and in ten cases out of a hundred the latent form eventually becomes active (contagious). And when this will happen, it is impossible to predict. [ 4 ]
Risk factors
The undisputed risk factors for the development of miliary tuberculosis are contact with patients and conditions that lead to immunosuppression – a weakening of the body’s immune defenses.
And the immune system is weakened:
- in HIV and AIDS, miliary tuberculosis is observed in 10% of patients with AIDS (see – Tuberculosis in HIV infection );
- with poor nutrition and chronic alcoholism;
- in cancer patients, including after chemotherapy;
- in chronic renal failure and continuous dialysis;
- due to antibody deficiency syndrome (hypogammaglobulinemia);
- in cases of long-term use of immunosuppressive drugs and corticosteroids.
Also, the risk of latent infection developing into active tuberculosis is increased in diabetes.
Pathogenesis
Tuberculosis is an insidious and complex disease, and despite the fact that the pathogenesis of M. tuberculosis is well known to phthisiologists, the exact mechanism of damage in its miliary forms has not been fully elucidated.
In individuals infected with mycobacteria that initially enter the body, the upper or posterior segments of the lung lobes are usually affected, and activation of alveolar macrophages leads to phagocytosis of the bacilli. That is, immunity limits their further reproduction, and usually with such an infection there are no clinical manifestations.
But even in the latent form, Ghon foci (primary tuberculosis complexes with encapsulated inactive bacteria) may also contain viable bacilli that are in a dormant state. And if immunity weakens, endogenous reactivation of M. tuberculosis occurs: they begin to multiply in macrophages, spreading to nearby cells and other organs by hematogenous means.
Foci in miliary tuberculosis have the appearance of homogeneous micronodes (1-3 mm in diameter) of a dense consistency, diffusely scattered throughout the lungs. [ 5 ]
In this case, destructive changes in the lungs in miliary tuberculosis are manifested in the form of tissue infiltration by these nodules, which can combine, forming larger foci of alteration and causing fibrosis of the lung tissue.
Symptoms miliary tuberculosis
The first signs of miliary tuberculosis are manifested by a deterioration in general condition and weakness.
The combination of symptoms, as well as signs of extrapulmonary localization of lesions, depend on the form of the disease.
Clinical forms of miliary tuberculosis include, first of all, miliary pulmonary tuberculosis, which is detected in 1-7% of patients with all forms of tuberculosis. Other typical symptoms of tuberculosis are also observed, in particular, night hyperhidrosis (increased sweating); loss of appetite and weight loss; cough (dry or with mucous sputum) and progressive dyspnea.
Most often, the manifestations of the disease are subacute or chronic; less often, acute miliary tuberculosis occurs.
In the acute course of generalized tuberculosis, chills and high hepatic fever (with temperature jumps) are observed; rapid heartbeat; difficulty breathing; cyanosis of the skin; nausea and vomiting (indicating intoxication), and impaired consciousness. This condition - due to some similarity with the symptoms of typhoid fever - can be defined as a typhoid form or typhoid miliary tuberculosis, which most often develops during primary infection.
In the extrapulmonary form of the disease, the infection can affect several organs at once. And then patients are diagnosed with miliary tuberculosis of multiple localization, which manifests itself in a variety of, often non-specific symptoms and leads to dysfunction of the affected organ or a certain organ system.
Thus, miliary tuberculosis of the liver may be asymptomatic, or it may be accompanied by fever and hyperhidrosis and lead to organ hypertrophy – hepatomegaly.
Also read:
- Intestinal tuberculosis
- Tuberculosis of the pancreas
- Tuberculosis of the kidneys
- Tuberculosis of the meninges (tuberculous meningitis)
One of the rarely diagnosed forms of tuberculosis of extrapulmonary localization is miliary tuberculosis of the skin, which in adults is considered a secondary form of the disease (the result of hematogenous spread of infection from the primary focus), and in childhood and adolescence - a primary form, with infection of the skin by contact. The most common areas of damage are the face, neck, extensor surfaces of the limbs and the trunk. Against the background of constitutional symptoms of tuberculosis, many small red nodules appear on the skin, which do not cause itching or pain, but very quickly turn into ulcers, so the diagnosis can be determined as miliary-ulcerative tuberculosis of the skin and subcutaneous tissues. [ 6 ]
Complications and consequences
Oxygen deficiency (respiratory distress syndrome) associated with pathological changes in the alveolar walls and impaired oxygen diffusion into the blood; pleural empyema with fibrothorax; formation of a bronchopleural fistula - complications of miliary tuberculosis of the lungs.
Miliary tuberculosis of the liver may be complicated by increased bilirubin levels in the blood and the development of jaundice, as well as fatty hepatosis and amyloid degeneration. Intestinal obstruction is the most common complication of miliary intestinal tuberculosis.
Meningeal miliary tuberculosis (the risk of which is increased in children) can lead to increased intracranial pressure, hydrocephalus and cranial nerve paralysis. The consequence of the generalized form of the disease is multiple organ failure. [ 7 ]
Diagnostics miliary tuberculosis
Early diagnosis helps to effectively treat miliary tuberculosis and reduce further transmission of the infection, but specialists examining tuberculosis patients acknowledge the existence of certain difficulties due to the many varieties of the disease and the non-specificity of the clinical manifestations of many forms.
Standard tests are required: isolation of M tuberculosis from sputum and bronchial lavage, PCR testing of tuberculosis bacillus DNA, analysis of adenosine deaminase levels in the blood, ESR. Histology of tissue biopsy samples is also performed. [ 8 ]
Read more:
- Laboratory diagnostics of tuberculosis
- Tuberculosis: Detection of Mycobacterium tuberculosis
- Methods for detecting tuberculosis
How is instrumental diagnostics carried out, the main method of which remains radiography, and ultrasound, high-resolution CT and MRI can be used to clarify the diagnosis, is detailed in the publication - Instrumental diagnostics of tuberculosis.
Miliary tuberculosis is visualized on chest X-ray by microfocal dissemination of both lungs - a cluster of multiple, clearly defined, diffuse fibronodular opacities. Some patients may have unilateral pleural effusion with thickening of the visceral and parietal pleura.
Differential diagnosis
Differential diagnostics is important: miliary pulmonary tuberculosis must be distinguished from cryptococcosis and sarcoidosis of the lungs, from malignant pleural mesothelioma; miliary tuberculosis of the brain - from meningococcal or staphylococcal meningitis; cutaneous miliary tuberculosis requires especially careful differentiation from dermatological diseases, from rashes in syphilis (tuberculous syphilides), etc.
More information in the materials:
Who to contact?
Treatment miliary tuberculosis
The main treatment for tuberculosis of any form is etiotropic, lasting 6-12 months; the main drugs are anti-tuberculosis antibacterial drugs: Isoniazid, Rifampicin, Macroside 500 (Pyrazinamide, Pyrazidine), Sodium para-aminosalicylate, etc.
Read more about their side effects, contraindications, methods of use and dosage in the publication - Tablets for tuberculosis.
In case of abscess formation of lesions and tissue necrosis, surgical treatment is performed.
Prevention
The main preventive measure is BCG vaccination or tuberculosis vaccination.
Also read:
In cases of detected latent infection, preventive treatment of tuberculosis is possible.
Forecast
Miliary tuberculosis is a life-threatening disease; fatal outcomes from miliary tuberculosis are observed in almost 27% of cases among adult patients, and in more than 15% of cases in children. [ 9 ], [ 10 ]
A favorable prognosis can only be achieved with the earliest possible detection of infection and effective antibiotic therapy.

