
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Lymph node tuberculosis: diagnosis, treatment
Medical expert of the article
Last reviewed: 12.07.2025
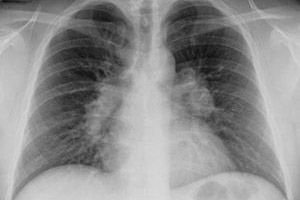
Today, tuberculosis of the lymph nodes is considered one of the most common forms of extrapulmonary tuberculosis, which can develop as a result of primary tuberculosis infection.
And the localization of pathological damage in the tissue of the lymph nodes – granulomatous inflammation – is explained by the lymphogenous route.
And the spread of this infection in the body.
Since lymph nodes (nodus lymphaticus) are a peripheral part of the branched lymphatic system, the definition of tuberculosis of peripheral lymph nodes, tuberculous peripheral lymphadenopathy is used; you can also come across the name "peripheral tuberculous lymphadenitis". Although the nature of the lesion of lymphoid tissue in lymphadenitis has a different pathogenesis and course, and the disease itself, according to ICD-10, belongs to infections of the skin and subcutaneous tissue (L04). While all forms of tuberculosis - and tuberculosis of the lymph nodes - are included in the class of infectious diseases (A15-A19).
Epidemiology
Statistics presented in the latest WHO Global Tuberculosis Report allow us to assess the state of the epidemic of this infection. In 2015, there were 10.4 million new cases of tuberculosis worldwide. Of these, 56% (5.9 million) were men; 34% (3.5 million) were women and 10% (1 million) were children. HIV-positive people accounted for 11% (1.2 million) of cases of detected tuberculosis.
The number of deaths in 2015 is estimated at 1.4 million, a 22% decrease compared to 2000.
Tuberculosis of the lymph nodes, as the main form of extrapulmonary tuberculosis, accounts for up to 5% of cases in European countries, about 10% in North America; in the endemic countries of the Indochina Peninsula and South Africa, this figure is 15-20% of all cases of tuberculosis (more than half are in AIDS patients).
In HIV-infected individuals, extrapulmonary tuberculosis develops in 68% of cases, and 45-60% of these are tuberculosis of the peripheral lymph nodes of various localizations.
Causes lymph node tuberculosis
The causes of tuberculosis of the lymph nodes are the penetration of the tuberculosis mycobacterium (Mycobacterium tuberculosis) or Koch's bacillus, which belongs to the class of actinobacteria, into the body.
How is tuberculosis of the lymph nodes transmitted? This bacterium, unable to move independently, but able to withstand heat, frost and lack of moisture, is most often transmitted from a sick person to a healthy person by coughing or sneezing, and this route of infection - airborne (aerogenic) - is the main one. Once in the lungs, the bacteria settle on the epithelium of the lower respiratory tract, and are then absorbed by alveolar macrophages (phagocytic cells) of the lung tissue. When macrophages fail to digest (lyse) the bacteria, a pulmonary form of the disease develops, which may also include tuberculosis of the peripheral lymph nodes, since the infectious agent enters the lymph through the intercellular fluid and settles in the lymphoid tissue of the lymph nodes, which act as a filter for the lymphatic fluid.
Phthisiatricians also believe that it is possible to become infected with tuberculosis through food (which has been contaminated with M. tuberculosis), for example, tuberculosis of the mesenteric lymph nodes can develop from consuming unpasteurized milk.
In addition, the infection is transmitted by contact, or it can be acquired in the womb of a mother who is a carrier of this bacterium.
Risk factors
The main risk factors are related to immune suppression that accompanies diseases such as gastric ulcers and diabetes, as well as to a decrease in the body's defenses due to alcoholism and drug addiction, the use of immune-suppressing drugs, and, of course, in patients with AIDS.
Pathogenesis
Tuberculosis of the peripheral lymph nodes is primary tuberculosis, since the lymph nodes are the first conductors of migration of immune cells for the introduction of Mycobacterium tuberculosis.
While studying the pathogenesis of lymph node damage by tuberculosis mycobacteria, researchers found that macrophages in the stroma of the lymph nodes absorb Koch's bacilli during chemotaxis, moving them into their cytoplasm (with part of their own plasma membrane).
After this, phagosomes (with absorbed mycobacteria) are formed in the lymphoid tissue, and from them – after merging with lysosomes (which contain digestive peroxide enzymes) – phagolysosomes are formed.
However, compared to most pathogenic microorganisms, M. tuberculosis have unique virulence factors: they exhibit increased resistance to phagocytosis, that is, the destructive effects of lysosomal enzymes, due to the characteristics of the cell membrane (containing lipid components), as well as a complex of alpha-, methoxy-, and keto-mycolic acids.
In addition, M. tuberculosis: has the UreC gene, which prevents an increase in the acidity level in phagosomes; blocks endosomal autoantigen molecules; produces the diterpene isotuberculosinol (isoTb), which prevents phagosome maturation.
Moreover, tuberculosis bacteria not only survive inside phagolysosomes, but also continue to multiply by replication, feeding on cholesterol, which is part of the cell membranes. Thus, due to their immunomodulatory effect, tuberculosis bacteria maintain their viability, which leads to the development of latent tuberculosis infection.
On the other hand, activation of cytokines (T-lymphocytes) and monocytes involved in the immune response contributes to the formation of specific phagocytic granulomas, which are formed from sedentary histiocytes (transformed macrophages). And granulotomatous lesions of the lymph nodes (often with caseous necrosis) are the main pathogenetic factor of tuberculosis of the peripheral lymph nodes.
By the way, relapse of tuberculosis of the lymph nodes is most often associated with the activation of the so-called L-forms of tuberculosis mycobacteria, which appear under the influence of antibacterial drugs (used in the treatment of all forms of tuberculosis) and are capable of existing for a long time in the body's cells.
Symptoms lymph node tuberculosis
According to clinical observations, symptoms of tuberculosis of the lymph nodes do not appear immediately, since the disease is slowly progressing (from 3 weeks to 8 months).
The first signs of tuberculosis of the cervical lymph nodes are non-specific and manifest themselves as painless swelling and some compaction. The affected node becomes clearly visible (reaches a size of up to 1-3 cm), elastic and mobile, but does not cause pain when pressed. However, during examination, 10-35% of patients experience pain. In 85% of cases, the lesion is unilateral.
Over time, the clinical picture is supplemented by pale skin; fever and chills; hyperhidrosis (heavy sweating); loss of appetite and weight loss; malaise and rapid fatigue. As the lesion progresses (with caseous necrosis), the skin in the lymph node area acquires a yellow or brownish tint. Blood tests show an accelerated ESR, an increase in the level of lymphocytes and plasma proteins, and a slight decrease in hemoglobin.
In tuberculosis of the intrathoracic lymph nodes, symptoms caused by intoxication (weakness, poor appetite, sweating during sleep, fever) predominate, and complaints of chest pain and cough appear when enlarged lymph nodes press on the bronchi. In children, phthisiatricians note an expansion of the peripheral venous network on the anterior chest wall (the Vidergoffer symptom indicates compression of the azygos vein); pain when pressing on the III-VI) thoracic vertebrae (indicates obvious inflammatory changes in the posterior mediastinum).
Read also – Symptoms of tuberculosis of the intrathoracic lymph nodes
In addition to fever, night sweats, and weakness, symptoms of mesenteric tuberculosis include nausea, vomiting, abdominal pain (lower right), bloating, constipation, or diarrhea. According to experts, clinically acute mesenteric tuberculosis manifests itself as acute appendicitis or acute gastroenteritis.
Symptoms of tuberculosis of the intra-abdominal lymph nodes also include fever, weight loss, and pain when touching the affected lymph node. And since the node is constantly growing, it can grow into nearby structures, forming adhesions.
Stages
There are four stages in the development of tuberculous peripheral lymphadenopathy.
The first stage begins with the moment of M. tuberculosis settling in the lymph node capsule until a granulotomatous focus is formed in the lymphoid tissue. As the granuloma grows, it occupies a significant part of the fibrous capsule of the node, which leads to an increase in the node and a pathological change in the structure of its tissues. This stage is usually called proliferative.
At the second stage, the walls of the granuloma capsule become thicker (due to the dystrophic transformation of extracellular matrix proteins into hyaline), and a necrotic zone forms in its center. The cheesy appearance of the dead cell mass determined the name of this stage of tuberculosis of the lymph nodes - caseous; at this stage, the pathological process may be accompanied by calcification of necrotic masses in the granuloma.
During the 3rd, abscessing stage, myomalacia (softening) of the granuloma contents occurs, turning it into something like pus (doctors call this a "cold abscess"). And the 4th stage is observed with superficially located large granulomas that break through the thinned skin, and then the pus comes out through a fistula, and a wound forms in its place.
Forms
In clinical phthisiology, types of tuberculosis of the lymph nodes are distinguished by their location.
Tuberculosis of the cervical lymph nodes can affect the anterior and posterior submandibular, postauricular and jugular lymph nodes, Virchow's nodes (in the supraclavicular fossa), paratracheal lymph nodes (on the anterior surface of the neck).
Tuberculosis of the intrathoracic lymph nodes - parietal and visceral - spreads to nodes localized in the lungs and along the bronchi (bronchopulmonary) and at the junction of the trachea and bronchi (tracheobronchial). This also includes a group of lymph nodes of the posterior mediastinum (located near the thoracic aorta) and mediastinal lymph nodes along the esophagus. Specialists note a more frequent lesion of bronchopulmonary hilar lymph nodes by M. tuberculosis. And although the infection does not spread directly to the lung tissue, they undergo significant changes due to the formation of infiltrates. The diagnosis may include tuberculous bronchoadenitis.
This localization of extrapulmonary tuberculosis infection accounts for up to two-thirds of all cases, and if tuberculosis of the lymph nodes develops in children, then 95% are this type of disease. More detailed information in the article - Tuberculosis of the intrathoracic lymph nodes in children
Tuberculosis of the intra-abdominal lymph nodes (intra-abdominal tuberculous lymphadenitis) includes tuberculosis of the mesenteric lymph nodes (intraperitoneal or mesenteric, often these are ileocecal lymph nodes) and tuberculosis of the retroperitoneal (retroperitoneal) nodes, which are located in the area of the spleen, portal and inferior vena cava, etc. The so-called mesenteric lymphadenopathy (or tuberculous mesenteric lymphadenitis) in most cases occurs with tuberculous lesions of the stomach or small intestine (i.e., it is a secondary form); its prevalence does not exceed 0.05% and is mostly detected in childhood and adolescence.
Complications and consequences
Pathological changes in lung tissue are noted as the main consequences and complications of tuberculosis of the intrathoracic lymph nodes. The most common complications are endobronchitis (sometimes with obstruction and atelectasis of a segment or lobe of the lung, which leads to respiratory failure) and interlobar pleurisy. There is also a risk of perforation of the caseous node and the release of its contents into the lumens of the bronchial tree, which is fraught with secondary infection of the pericardial lymph nodes.
In case of tuberculosis of the intra-abdominal lymph nodes, complications may include the formation of ulcers, intestinal obstruction or partial intestinal obstruction, varicose veins of the abdominal veins, ascites, tuberculous peritonitis, etc.
Diagnostics lymph node tuberculosis
Today, the diagnosis of tuberculosis of the lymph nodes, in addition to anamnesis and examination, includes blood tests: clinical and biochemical (including the level of T-lymphocytes).
An intradermal tuberculin test (Mantoux test) is mandatory. More details in the publication - Tuberculosis: detection of Mycobacterium tuberculosis
Instrumental diagnostics include radiography, ultrasound, CT, and in some cases MRI. Excisional biopsy of the inflamed lymph node is used for subsequent histomorphological examination of its contents. In the case of deeply located affected lymph nodes, the method of choice may be endoscopic ultrasound examination with biopsy.
Tuberculous lesions of the mesenteric lymph nodes, even with X-ray examination, are very similar to kidney or gallstones, and uro- or cholangiography is often required. And in case of particularly large granulotomatous lesions of the lymph nodes in the mesentery (up to 8-10 cm in diameter), laparotomy may be required.
Given the high virulence of M. tuberculosis, the role of differential diagnostics of this disease is difficult to overestimate. For example, lymphadenopathy of the neck (lymphadenitis) caused by atypical mycobacteria (Mycobacterium scrofulaceum) and other pathogens (Streptococcus pyogenes, Staphylococcus aureu, etc.) should be excluded.
What tests are needed?
Differential diagnosis
Differential diagnostics of tuberculosis localized in the intrathoracic lymph nodes is designed to distinguish it from lymph node hyperplasia, lymphogranulomatosis, lymphocytic leukemia, manifestations of lung cancer, metastasis of carcinoma, tumors and cysts of the thymus gland or bronchi, teratoma, sarcoidosis, etc.
Tuberculosis of the intra-abdominal lymph nodes can mimic a number of other abdominal disorders, such as pancreatic cancer, node metastases, and lymphoma. It can be difficult for physicians to differentiate mesenteric lymph node tuberculosis from chronic appendicitis, ileocecal lymph node cancer, and Burkitt's lymphoma.
Tuberculosis of the lymph nodes of intra-abdominal localization may look like a cyst or malignant neoplasm of the pancreas, which creates serious diagnostic problems.
Who to contact?
Treatment lymph node tuberculosis
It should be noted right away that treatment of tuberculosis of the lymph nodes can be medicinal or surgical. Doctors claim that no compresses will help with tuberculosis of the lymph nodes, and recommend taking vitamins (they will be useful).
The first-line anti-tuberculosis drugs used in combination therapy for this disease include the following medications:
Isoniazid (Isonizide, Tubazid, Dinacrine, Pyrazidine, Eutizone and other trade names) is administered intramuscularly or intravenously, and tablets (100, 200 and 300 mg) are taken orally at a rate of 5-15 mg per kilogram of body weight per day (in three doses during the day). The duration of the course of treatment is determined by the doctor. There may be side effects in the form of headache, nausea and vomiting, urticaria, insomnia, deterioration of liver function, pain along the peripheral nerves and paresthesia. This drug is not prescribed for epilepsy, liver and thyroid problems, atherosclerosis, bronchial asthma, skin autoimmune diseases.
The antibiotic Rifampicin (Rifampin, Riforal, Ripamisin Benemetsin, Tubotsin) is prescribed at 450 mg once a day (an hour before meals). Side effects include dyspepsia, dysfunction of the pancreas and liver, and a decrease in leukocytes in the blood. And the list of contraindications includes kidney pathologies, pregnancy, and early childhood.
The anti-tuberculosis drug Sodium para-aminosalicylate (PAS sodium salt) in powder form for solution preparation is usually taken two sachets a day (no more than 12 g), dissolving the powder in warm water (half a glass per single dose). This drug is contraindicated in kidney inflammation, hepatitis and cirrhosis of the liver, ulcerative diseases of the gastrointestinal tract (it is undesirable to take it if you have problems with the thyroid gland); and its side effects include loss of appetite, nausea and vomiting, abdominal pain, bronchial spasm, joint pain.
Calcium benzamidosalicylate (Bepask) in powder or tablet form is used in the same way.
Surgical treatment
Surgical treatment of tuberculosis of the lymph nodes involves the removal of the contents of the granulotomatous formation in the lymph node after its opening, followed by disinfection and (if necessary) drainage.
Western phthisiologists use such a surgical method as excision of tuberculous lymph nodes, but only in exceptional cases and in accessible places. Also, affected nodes on the neck can be removed either by repeated aspiration or curettage (scraping).
However, as experience shows, excision should be considered as an addition to antibiotic therapy. For example, removal of the parotid lymph node affected by tuberculosis mycobacteria quite often leads to a relapse of tuberculosis of the lymph nodes, and also provokes the spread of infection to other organs. In addition, when removing cervical lymph nodes, there is a risk of damage to the facial nerve
So the most effective treatment is considered to be traditional antibiotic treatment – for two to three months.
Prevention
The main prevention is BCG vaccination. Read all the details in the article - Sanitary and social prevention of tuberculosis


 [
[