
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Helicobacter
Medical expert of the article
Last reviewed: 04.07.2025
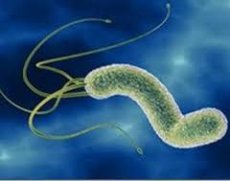
Helicobacter pylori was discovered in 1982 by B. Marshall and R. Warren during a study of gastric mucosa biopsies. The genus Helicobacter currently includes more than 10 species, some of which were previously included in the genus Campylobacter.
 [ 1 ], [ 2 ], [ 3 ], [ 4 ], [ 5 ], [ 6 ], [ 7 ], [ 8 ], [ 9 ]
[ 1 ], [ 2 ], [ 3 ], [ 4 ], [ 5 ], [ 6 ], [ 7 ], [ 8 ], [ 9 ]
Morphology of Helicobacter
H. pylori is somewhat larger than other species (0.5-1.0 x 2.5-5 μm) and has the shape of a rod, spiral or "ox bow". Lophotrich (up to 5 flagella) or monotrich, sometimes both forms are present in the population. On agar media it is slightly mobile or mobile. It grows on media for campylobacter, but grows better on "chocolate" agar, forming colonies with a diameter of 0.5-1.0 mm on it in 2-7 days. Weak a-hemolysis is observed on 10% blood agar. Microaerophilic conditions or an atmosphere enriched with CO2 are required for growth. The bacteria do not grow in aerobic or anaerobic conditions.
Biochemical properties of Helicobacter
H. pylori is oxidase- and catalase-positive; does not form hydrogen sulfide, does not hydrolyze hippurate, has high urease activity. Resistant to triphenyltetrazolium chloride at a concentration of 0.4-1.0 mg/ml; resistant to 0.1% sodium selenite solution, to a lesser extent - to 1% glycine.
Helicobacter pathogenicity factors
The virulence factors of H. pylori are motility; urease (neutralizes HCl and damages epithelial cells); protein cytotoxin, which causes vacuolization of epithelial cells and damages intercellular bridges; lipopolysaccharide; proteinase; lipase; catalase, hemolysin, etc.
Epidemiology of Helicobacter pylori
Infection of humans most likely occurs via the fecal-oral mechanism. The pathogen, penetrating through mucin into the submucosa of the stomach, colonizes epithelial cells, often penetrating into them. Progressive focal inflammation leads to the development of gastritis, peptic ulcers of the stomach and duodenum. Further development of gastric adenocarcinoma or lymphoma (Mucosa Associated Lymphoid Tissue Lymphoma) may occur.
Treatment of helicobacteriosis
The most effective drug for the treatment of chronic gastritis and gastric ulcer or duodenal ulcer is DeNol (colloidal bismuth subcitrate), which selectively acts only on H. pylori, which is combined with trichopolum (metronidazole) and amoxicillin (or clarithromycin) to enhance the therapeutic effect.

