Medical expert of the article
New publications
Nodular periarteritis
Last reviewed: 13.05.2022

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
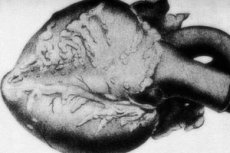
A rare pathology - periarteritis nodosa - is accompanied by lesions of medium and small-caliber arterial vessels. In the vascular walls, processes of connective tissue disorganization, inflammatory infiltration and sclerotic changes occur, resulting in clearly marked aneurysms.[1]
Other names for the disease: polyarteritis , necrotizing arteritis, panarteritis.
Epidemiology
Periarteritis nodosa is a systemic pathology, necrotizing vasculitis, damaging the medium and small arterial vessels of the muscular type. Most often, the disease spreads to the skin, kidneys, muscles, joints, peripheral nervous system, digestive tract, and other organs, less often the lungs. Pathology usually manifests itself initially with general symptoms (fever, general deterioration of well-being), then more specific signs join.
The most common methods for diagnosing the disease are biopsy and arteriography.
The most acceptable medications for treatment are glucocorticoid drugs and immunosuppressants.
The frequency of detection of periarteritis nodosa is from two to thirty cases per 1 million patients.
The average age of the patients is 45-60 years. Men are more often ill (6:1). In women, the disease occurs more often according to the asthmatic type, with the development of bronchial asthma and hypereosinophilia.
Approximately 20% of patients diagnosed with periarteritis nodosa have hepatitis (B or C).[2], [3]
Causes of the periarteritis nodosa
Scientists have not yet found a clear cause for the development of periarteritis nodosa. However, the following main triggers of the disease are distinguished:
- reaction to medication;
- persistent viral infection (hepatitis B).
Experts have compiled a rather impressive list of drugs involved in the development of periarteritis nodosa. Among these medicines:
- beta-lactam antibiotics;
- macrolide preparations;
- sulfa drugs;
- quinolones;
- antiviral agents;
- sera and vaccines;
- selective serotonin reuptake inhibitors (fluoxetine);
- anticonvulsants (phenytoin);
- Levodopa and Carbidopa;
- thiazides and loop diuretics;
- Hydralazine, Propylthiouracil, Minocycline, etc.
Every third or fourth patient with periarteritis nodosa had hepatitis B surface antigen (HBsAg) or immunocomplexes with it. Other hepatitis B antigens (HBeAg) and antibodies to the HBcAg antigen formed during viral replication were also determined. It is noteworthy that the incidence of periarteritis nodosa in France has decreased significantly over the past decades, thanks to the widespread vaccination against hepatitis B.[4]
Also, approximately one in ten patients has a hepatitis C virus, but scientists have not yet proven the intricacies of the relationship. Other viral infections are also “under suspicion”: human immunodeficiency virus, cytomegalovirus, rubella and Epstein-Barr viruses, type I T-lymphotropic virus, parvovirus B-19, etc.
There are all prerequisites for suggesting the involvement of vaccination against hepatitis B and influenza in the development of periarteritis nodosa.
An additional suggested factor is genetic predisposition, which also requires evidence and further study.[5]
Risk factors
Periarteritis nodosa is a little-studied disease, but even now experts consider it polyetiological, since many causes and factors may be involved in its development. Often, a relationship is found with focal infections: streptococcal, staphylococcal, mycobacterial, fungal, viral, etc. Human hypersensitivity to certain medications, for example, to antibiotics and sulfonamides, plays a significant role. However, in many cases, even with a thorough diagnosis, the etiological factor cannot be identified.[6]
Here are some of the risk factors doctors are aware of today:
- age category over 45 years old, as well as children from 0 to 7 years old (genetic factor);
- sudden changes in temperature, hypothermia;
- excessive exposure to ultraviolet radiation, abuse of sunburn;
- excessive physical and mental overload;
- any damaging effects, including trauma or surgery;
- hepatitis and other liver diseases;
- metabolic disorders, diabetes mellitus;
- hypertension;
- administration of vaccines and persistence of HbsAg in blood serum.
Pathogenesis
The pathogenesis of the occurrence of periarteritis nodosa consists in the formation of a hyperallergic response of the body to the influence of etiological factors, in the development of an autoimmune reaction of the antigen-antibody type (in particular, to the walls of blood vessels), in the formation of immunocomplexes.
Since endothelial cells are equipped with receptors for the IgG Fc fragment with the first complement fraction Clq, the mechanisms of interaction between immunocomplexes and vessel walls are facilitated. There is a deposition of immunocomplexes in the vascular walls, which entails the development of an immune inflammatory process.
The formed immunocomplexes stimulate complement, which leads to damage to the walls and the formation of chemotactic components that attract neutrophils to the damaged area.[7]
Neutrophils perform a phagocytic function in relation to immunocomplexes, but at the same time lysosomal proteolytic enzymes are released that damage the walls of blood vessels. In addition, neutrophils “stick” to the endothelium and, in the presence of complement, release active oxygen radicals that provoke vascular damage. At the same time, the endothelial release of factors favoring increased blood clotting and the formation of blood clots in the affected vessels is potentiated.[8]
Symptoms of the periarteritis nodosa
Periarteritis nodosa reveals itself to be common non-specific manifestations: a person has a constantly elevated temperature, he is progressively losing weight, pain in muscles and joints is disturbing.
An increase in temperature in the form of persistent fever is characteristic of 98-100% of cases: the temperature curve is of the wrong type, there is no response to antibiotic therapy, but corticosteroid therapy is effective. The temperature may subsequently normalize, against the background of the development of multiple organ pathology.
The emaciation of patients is pathognomic. In some patients, weight is reduced by 35-40 kg within a few months. At the same time, the degree of thinness exceeds that in oncopathologies.
Pain in the muscles and joints is especially characteristic of the initial stage of nodular periarteritis. Soreness especially often affects large joints and calf muscles.[9]
Multiple organ pathologies are divided into several types, which determines the symptoms of the disease:
- With damage to the renal vessels (and this occurs in most patients), an increase in blood pressure is noted. Hypertension is persistent, persistent, causing a severe degree of retinopathy. Loss of visual function is possible. Urinalysis reveals proteinuria (up to 3 g/day), micro or macrohematuria. In some cases, the vessel expanded by the aneurysm ruptures, forming a perirenal hemorrhage. Renal failure develops during the first three years of the disease.
- If the vessels located in the abdominal cavity are damaged, the symptoms appear already at an early stage of periarteritis nodosa. The main symptoms are abdominal diffuse pain, persistent and progressive. Dyspeptic disorders are noted: diarrhea mixed with blood up to ten times a day, emaciation, bouts of nausea and vomiting. If ulcerative perforation occurs, signs of acute peritonitis develop. There is a risk of gastrointestinal bleeding.
- With damage to the coronary vessels, pain in the heart is not typical. There are heart attacks, mostly small-focal character. The phenomena of cardiosclerosis are rapidly increasing, which entails the appearance of arrhythmias, signs of cardiac insufficiency.
- When the respiratory system is affected, bronchospasm, hypereosinophilia, and eosinophilic infiltrates in the lungs are found. The formation of vascular inflammation of the lungs is characteristic: the disease is accompanied by cough, scanty sputum discharge, less often - hemoptysis, aggravated by symptoms of insufficient respiratory function. On the radiograph, a sharply enhanced vascular pattern is visualized in the form of a congestive lung, infiltration of the lung tissue (mainly in the basal region).
- When the peripheral nervous system is involved in the process, asymmetric poly and mononeuritis is noted. The patient is worried about severe pain, numbness, sometimes muscle weakness. The legs are more commonly affected, less often the arms. Some patients develop polymyeloradiculoneuritis, paresis of the feet and hands. Often, peculiar nodules are found along the trunks of blood vessels, ulcers and foci of necrosis of the skin. Possible necrosis of soft tissues and the development of gangrenous complications.
First signs
The initial clinical picture of periarteritis nodosa reveals itself as fever, feeling very tired, increased night sweats, loss of appetite and emaciation, muscle weakness (especially felt in the limbs). Many patients develop muscle pain, accompanied by focal ischemic myositis and joint pain. The affected muscles lose their strength, the development of inflammatory processes in the joints is possible.[10]
The severity of the first signs is different, which depends to a greater extent on which organ or organ system is affected:
- defeat of the peripheral nervous system is manifested by motor and sensory disorders of the ulnar, median and peroneal nerves, it is also possible to develop distal symmetrical polyneuropathy;
- the central nervous system responds to the pathology with headaches, strokes (ischemic and hemorrhagic) are less common against the background of high blood pressure;
- kidney damage is manifested by arterial hypertension, a decrease in the daily amount of urine, uremia, general changes in urine sediment, the appearance of blood and protein in the urine in the absence of cellular casts, back pain, and in severe cases - signs of kidney failure;
- the digestive tract makes itself felt with pain in the liver and abdomen, nausea, vomiting, diarrhea, symptoms of malabsorption, intestinal perforation and peritonitis;
- from the side of the heart, there may be no pathological signs, or symptoms of heart failure appear;
- on the skin there is a livedo reticularis, reddening painful nodules, a rash in the form of vesicles or vesicles, areas of necrosis and ulcerative lesions;
- the genitals are affected by the type of orchitis, the testicles become painful.
Kidney damage in nodular periarteritis
The kidneys are affected in more than 60% of patients with periarteritis nodosa. Moreover, in more than 40% of cases, the lesion is a renal failure.
The likelihood of developing kidney disorders depends on the gender and age category of patients, on the presence of pathologies of the skeletal muscles, the valvular system of the heart and the peripheral nervous system, on the type of course and phase of the disease, on the presence of viral hepatitis antigen and cardiovascular values.
The rate of development of nephropathy is directly determined by the level of C-reactive protein and rheumatoid factor in the blood.
Renal disorders in periarteritis nodosa are due to stenosis and the appearance of microaneurysms of the renal vessels. The degree of pathological changes correlates with the severity of disorders of the nervous system. It must be understood that kidney damage dramatically reduces the chances of survival of patients. However, this issue of the influence of certain disorders of renal function on the course of periarteritis nodosa has not been studied enough.
The inflammatory process usually extends to interlobar arterial vessels and less often to arterioles. Presumably, glomerulonephritis is uncharacteristic of periarteritis nodosa and occurs mainly against the background of microscopic angiitis.
The rapid aggravation of renal failure is due to numerous heart attacks in the kidneys.[11]
Heart failure
The picture of the defeat of the cardiovascular apparatus is noted in every second case out of ten. Pathology is manifested by hypertrophic changes in the left ventricle, increased heart rate, and cardiac arrhythmias. Inflammation of the coronary vessels in periarteritis nodosa can provoke the appearance of angina pectoris and the development of myocardial infarction.
In macropreparations, in more than 10% of cases, nodular thickenings of the type of a rosary are found, from a few millimeters to a couple of centimeters in diameter (up to 5.5 cm in case of damage to large vascular trunks). The section shows an aneurysm, often with thrombotic filling. The final diagnostic role is played by histology. A typical feature of periarteritis nodosa is a polymorphic vascular lesion. There is a combination of different types of connective tissue disorganization:[12]
- mucoid swelling, fibrinoid changes with further sclerosis;
- narrowing of the vascular lumen (up to obliteration), the formation of blood clots, aneurysms, in severe cases - rupture of blood vessels.
Vascular changes become a trigger in the development of necrosis, atrophic and sclerotic processes, hemorrhages. Some patients have phlebitis.
In the heart, atrophy of the fatty layer of the epicardium, brown myocardial dystrophy, and in hypertension, left ventricular hypertrophy are found. With coronary lesions, focal myocardial necrosis, dystrophy and atrophy of muscle fibers develop. Myocardial infarctions are relatively rare - mainly due to the formation of collateral blood flow. Thrombosculitis is found in the coronary arterial trunks.[13]
Skin manifestations of periarteritis nodosa
Skin signs of the disease are observed in every second patient with periarteritis nodosa. Often the appearance of rashes becomes the first, or one of the first signs of a violation. Typical symptoms are:
- vesicular and bullous rash;
- vascular papulo-petechial purpura;
- sometimes - the appearance of subcutaneous nodular elements.
In general, the skin manifestations of periarteritis nodosa are heterogeneous and varied. General signs may be:
- the nature of the rash is inflammatory;
- the rash is symmetrical;
- there is a tendency to swelling, necrotic changes and hemorrhages;
- at the initial stage, the rash is localized in the region of the lower extremities;
- evolutionary polymorphism is noted;
- there is a connection with pre-existing infections, medication, temperature changes, allergic processes, autoimmune pathologies, impaired venous circulation.
Skin lesions vary in variety, ranging from macules, nodules, and purpura to necrosis, ulcers, and erosions.
Nodular periarteritis in children
Juvenile polyarteritis is a form of polyarteritis nodosa that is found predominantly in pediatric patients. This variant of the course of the disease is distinguished by a hyperergic component, most of the peripheral vessels are damaged, there is a considerable risk of developing thromboangiitis complications in the form of dry tissue necrosis, gangrenous processes. Visceral disorders are relatively weak and do not affect the outcome of the pathology, but there is a tendency to a long course with periodic relapses.
The classic form of juvenile polyarteritis has a severe course: kidney damage, high blood pressure, abdominal ischemia, cerebral vascular crises, inflammation of the coronary vessels, pulmonary vasculitis, and numerous mononeuritis are noted.
Among the causes of the disease are considered mainly allergic and infectious factors. The classic form of periarteritis nodosa is associated with a viral infection of hepatitis B. Often the onset of the disease is noted along with acute respiratory viral infections, otitis and tonsillitis, somewhat less often with the introduction of vaccines or drug therapy. A genetic predisposition is not excluded either: often, rheumatological, allergic or vascular pathologies are found in the direct relatives of a sick child.
The incidence of periarteritis nodosa in childhood is unknown: the disease is diagnosed very rarely.
Pathogenesis is often due to immunocomplex processes with an increase in complement activity and leukocyte accumulation in the area of fixation of immunocomplexes. An inflammatory reaction occurs in the walls of small-caliber and medium-caliber arterial trunks. As a result, proliferative-destructive vasculitis develops, the vascular bed is deformed, blood circulation is inhibited, the rheological and coagulation properties of blood are disturbed, thrombosis and tissue ischemia are noted. Gradually, wall fibrosis is formed, aneurysms with a diametrical size of up to 10 mm are formed.
Stages
Periarteritis nodosa can take place in the acute, subacute and chronic recurrent stages.
- The acute stage is characterized by a short initial period, with intense generalization of vascular lesions. The course of the disease is severe from the moment of its onset. The patient has a high temperature of the type of remitting fever, profuse sweating, severe joint pain, myalgia, abdominal pain. With the defeat of the peripheral circulation, a rapid formation of wide foci of skin necrosis occurs, and a distal gangrenous process develops. With damage to internal organs, intense vascular-cerebral crises, myocardial infarction, polyneuritis, and intestinal necrosis are noted. The acute period can be traced for 2-3 months or more, up to one year.
- The subacute stage begins gradually, mainly in patients with predominant localization of the pathological process in the area of the internal organs. For several months, subfebrile temperature is fixed in patients, or the temperature periodically rises to high rates. There is progressive emaciation, joint and headaches. Subsequently, there is an acute development of a cerebrovascular crisis, or abdominal syndrome, or polyneuritis. The pathology remains active for up to three years.
- The chronic stage can be observed in both acute and subacute disease processes. Patients begin alternating periods of exacerbation and disappearance of symptoms. During the first few years, relapses occur every six months, then remissions may become longer.
Acute nodular periarteritis
The acute phase of periarteritis nodosa usually proceeds severely, since certain vital organs are affected. In addition to clinical manifestations, the assessment of disease activity is also influenced by indicators of laboratory changes, although they are not specific enough. There may be an increased ESR, eosinophilia, leukocytosis, an increase in gamma globulins and the amount of CEC, a decrease in the level of complement.
Periarteritis nodosa is characterized by either a fulminant course or periodic acute phases against the background of constant progression of the pathology. A lethal outcome can occur almost at any time with the development of renal or cardiovascular failure, damage to the digestive tract (perforated intestinal infarction is especially life-threatening). The disorder of the kidneys, heart and central nervous system is often exacerbated by persistent arterial hypertension, which leads to serious late complications, which can also cause the death of the patient. In the absence of treatment, the five-year survival rate is estimated at about 13%.[14]
Complications and consequences
The severity of the patients' condition and the likelihood of complications are due to a steady increase in blood pressure, up to 220/110-240/170 mm Hg. Art.
The active stage of the disease often ends with cerebral circulatory disorders. The progression of the pathology leads to the fact that hypertension becomes malignant, cerebral edema occurs, in some patients chronic renal failure develops, cerebral hemorrhage and kidney rupture.
Often, a renal syndrome is formed, ischemia of the juxtaglomerular renal apparatus develops, and the mechanism of the renin-angiotensin-aldosterone system is disrupted.
On the part of the digestive tract, the development of local and diffuse ulcers, foci of necrosis and intestinal gangrene, inflammation of the appendix is noted. Patients have an intense abdominal pain syndrome, intestinal bleeding may develop, signs of peritoneal irritation appear. Intraintestinal inflammatory disorders do not have histological signs of ulcerative colitis. There may be internal bleeding, pancreatitis with pancreonecrosis, infarction of the spleen and liver.
Damage to the nervous system can be complicated by the development of a cerebral vascular crisis, which manifests itself abruptly, with headache and vomiting. Then the patient loses consciousness, clonic and tonic convulsions, sudden hypertension are noted. After an attack, lesions often appear in the brain, which is accompanied by gaze paralysis, diplopia, nystagmus, facial asymmetry, and visual impairment.
In general, periarteritis nodosa is a life-threatening pathology and requires the earliest possible diagnosis and aggressive permanent treatment. Only under such conditions is it possible to achieve stable remission and avoid the development of severe dangerous consequences.
Outcome of nodular periarteritis
More than 70% of patients with periarteritis nodosa have an increase in blood pressure and the development of signs of progressive renal failure within the first 60 days from the onset of the disease. Damage to the nervous system is possible, with preservation of sensitivity, but limitation of motor activity.
The vessels of the abdominal cavity may become inflamed, resulting in severe abdominal pain. Dangerous complications often become ulcers of the stomach and intestines, gallbladder necrosis, perforation and peritonitis.
Coronary vessels are affected less frequently, but the following outcome is also possible: patients develop myocardial infarction. When the blood vessels are damaged, strokes occur.
In the absence of treatment, almost all patients die during the first few years from the onset of the pathology. The most common problems leading to death: extensive arteritis, infectious processes, heart attack, stroke.
Diagnostics of the periarteritis nodosa
Diagnostic measures begin with the collection of complaints from the patient. Particular attention is drawn to the presence of rashes, the formation of necrotic foci and ulcerative skin lesions, pain in the area of the rash, in the joints, body, limbs, muscles, as well as general weakness.
An external examination of the skin and joints is mandatory, the location of the rashes and the zone of soreness is assessed. Lesions are carefully palpated.
To assess the level of disease activity, laboratory tests are performed:
- general clinical detailed blood test;
- general therapeutic biochemical blood test;
- assessment of the level of serum immunoglobulins in the blood;
- study of the level of complement with its fractions in the blood;
- assessment of the concentration of C-reactive protein in blood plasma;
- determination of rheumatoid factor;
- general examination of the urinary fluid.
With periarteritis nodosa, hematuria, cylindruria and proteinuria are found in the urine. A blood test reveals neutrophilic leukocytosis, anemia, and thrombocytosis. The biochemical picture is represented by an increase in the fractions of γ and α2-globulins, fibrin, sialic acids, seromucoid, C-reactive protein.
Instrumental diagnostics is carried out to clarify the diagnosis. In particular, a musculoskeletal biopsy is performed: in the biomaterial taken from the lower leg or anterior abdominal wall, inflammatory infiltrates and necrosis zones in the vessel walls are found.
Periarteritis nodosa is often accompanied by aneurysmal vascular changes that are visible during examination of the fundus.
Doppler ultrasound of the renal vessels helps to determine their stenosis. Plain chest radiography visualizes an increase in the pattern of the lungs and a violation of its configuration. An electrocardiogram and ultrasound examination of the heart can detect cardiopathy.
A micropreparation that can be used for study is the mesenteric artery in the exudative or proliferative stage of arteritis, subcutaneous tissue, sural nerve and muscles. Liver and kidney specimens may give a false negative result due to sampling error. In addition, such a biopsy can cause bleeding from undiagnosed microaneurysms.
A macropreparation in the form of excised pathologically altered tissue is fixed in a solution of ethanol, chlorhexidine, formalin for further histological examination.
A biopsy of tissue that is not affected by pathology is not advisable, since periarteritis nodosa has a focal character. Therefore, tissue is taken for biopsy, the defeat of which is confirmed by a clinical study.
If the clinical picture is minimal or absent, then electromyography and nerve conduction assessment procedures can identify the area of the proposed biopsy. In case of damage to the skin, it is preferable to remove biomaterial from deep layers or PZhK, excluding the surface layers (demonstrate erroneous indicators). Testicular biopsy is also often inappropriate.
Diagnostic criteria
The diagnosis of periarteritis nodosa is made based on the anamnesis data, on the characteristic symptoms, on the results of laboratory diagnostics. It is worth noting that changes in laboratory parameters are nonspecific, since they mainly reflect the stage of pathology activity. Given this, experts distinguish the following diagnostic criteria for the disease:
- Pain in the muscles (especially in the lower extremities), general weakness. Diffuse myalgia, not affecting the area of the lower back and shoulders.
- Pain in the testicles, not related to infectious processes or traumatic injuries.
- Uneven cyanosis on the skin of the limbs and body, like livedo reticularis.
- Weight loss of more than 4 kg, which is not associated with diets and other dietary changes.
- Polyneuropathy or mononeuritis with all neurological signs.
- An increase in diastolic blood pressure above 90 mm Hg. Art.
- An increase in blood urea (more than 14.4 mmol / liter - 40 mg%) and creatinine (more than 133 μmol / liter - 1.5 mg%), which is not related to dehydration or urinary tract obstruction.
- The presence of HBsAg, or the corresponding antibodies in the blood (viral hepatitis B).
- Vascular changes on the arteriogram in the form of aneurysms and occlusions of visceral arterial vessels, without connection with atherosclerotic changes, fibromuscular dysplastic processes and other non-inflammatory pathologies.
- Detection of granulocytic and mononuclear cell infiltration of vascular walls during morphological diagnostics of biomaterial taken from arterial vessels of small and medium caliber.
Confirmation of at least three criteria makes it possible to make a diagnosis of periarteritis nodosa.
Classification
There is no generally accepted classification of nodular periarteritis. Specialists usually systematize the disease according to etiological and pathogenetic characteristics, according to histological features, severity of the course, and clinical picture. The vast majority of practitioners use a morphological classification based on clinical changes in tissues, on the depth of localization and the caliber of damaged vessels.
The following clinical types of the disease are divided:
- The classic variant (renal-visceral, renal-polyneuritic) is characterized by damage to the kidneys, central nervous system, peripheral nervous system, heart and digestive tract.
- Monoorgan-nodular variant - a mild type of pathology, manifested by visceropathy.
- The dermato-thrombangic variant is a slowly progressive form, which is accompanied by an increase in blood pressure, the development of neuritis, and impaired peripheral blood flow due to the appearance of nodules along the vascular lumen.
- Pulmonary (asthmatic) variant - manifested by changes in the lungs, bronchial asthma.
According to the international classification ICD-10, nodular vascular inflammation occupies class M30 with the following distribution:
- M30.1 - allergic type with lung damage.
- M30.2 - juvenile type.
- M30.3 - changes in the mucous tissues and kidneys (Kawasaki syndrome).
- M30.8 - other conditions.
According to the nature of the course of nodular periarteritis, the following forms of pathology are divided:
- The fulminant form is a malignant process in which the kidneys are affected, thrombosis of the intestinal vessels occurs, necrosis of the intestinal loops. The prognosis is especially negative, the patient dies within one year from the onset of the disease.
- The fast form does not proceed too rapidly, but otherwise has much in common with the fulminant course. Survival is poor, often patients die from sudden rupture of the renal artery.
- The recurrent form is characterized by the suspension of the disease process as a result of the treatment. However, the growth of pathology resumes with a decrease in the dosage of drugs, or under the influence of other provoking factors - for example, against the background of the development of an infectious-inflammatory process.
- The slow form is most often thromboangitic. It extends to peripheral nerves and the vasculature. The disease can gradually increase its intensity over a decade or even more, provided there are no serious complications. The patient becomes disabled, he needs constant ongoing treatment.
- The benign form is considered the mildest variant of periarteritis nodosa. The disease proceeds in isolation, the main manifestations are found only on the skin, there are long periods of remission. The survival rate of patients is relatively high - subject to competent and regular therapy.
Clinical guidelines
The diagnosis of periarteritis nodosa should be substantiated by the relevant clinical manifestations and laboratory diagnostic data. Positive biopsy values are important for confirming the disease. The earliest possible diagnosis is necessary: urgent-aggressive therapy should be started before the pathology spreads to vital organs.
Clinical symptoms in periarteritis nodosa are distinguished by pronounced polymorphism. Symptoms of the disease with and without HBV are similar. The most acute development is typical for the pathology of drug genesis.
Patients with suspected periarteritis nodosa are recommended to perform a histology that reveals a typical picture of focal necrotizing arteritis with mixed cell infiltration in the vessel wall. The most informative is considered a biopsy of skeletal muscles. During the biopsy of the internal organs, the risk of internal bleeding increases significantly.
To determine the treatment tactics, patients with periarteritis nodosa should be divided according to the severity of the pathology, as well as the refractory type of the course of the disease, which is not characterized by a reverse symptomatic development, or even an increase in clinical activity in response to a one and a half month classical pathogenetic therapy.
Differential diagnosis
Periarteritis nodosa is primarily differentiated from other known systemic pathologies affecting the connective tissue.
- Microscopic polyarteritis is a form of necrotizing vasculitis that affects capillary vessels, as well as venules and arterioles, with the formation of anti-neutrophil antibodies. For the disease, the appearance of glomerulonephritis is typical, a late gradual increase in blood pressure, rapidly increasing renal failure, the development of necrotizing alveolitis and pulmonary hemorrhage.
- Wegener's granulomatosis is accompanied by the development of tissue destructive changes. Ulcers appear on the mucous tissue of the nasal cavity, the nasal septum is perforated, and lung tissue disintegrates. Anti-neutrophil antibodies are often detected.
- Rheumatoid vasculitis is characterized by the appearance of trophic ulcerative lesions on the legs, the development of polyneuropathy. During the diagnosis, the degree of the articular syndrome is necessarily assessed (the presence of erosive polyarthritis with a violation of the configuration of the joints), a rheumatoid factor is detected.
In addition, skin manifestations similar to periarteritis nodosa appear on the background of septic embolism, left atrial myxoma. It is important to exclude septic conditions even before the use of immunosuppressants for the treatment of periarteritis nodosa.
A combination of symptoms such as polyneuropathy, fever, polyarthritis is found in patients with Lyme disease (another name is borreliosis). To exclude the disease, it is necessary to trace the epidemiological history. Moments that allow you to suspect borreliosis are as follows:
- tick bites;
- visits to natural focal zones during the period of special tick activity (late spring - early autumn).
To make a diagnosis, a blood test is performed to check for the presence of antibodies to Borrelia.
Who to contact?
Treatment of the periarteritis nodosa
Treatment should be as early and prolonged as possible, with the appointment of an individual therapeutic regimen, depending on the severity of clinical symptoms and the stage of periarteritis nodosa.
In the acute period, bed rest is mandatory, which is especially important if the pathological foci of periarteritis nodosa are located on the lower extremities.
The approach to treatment is always complex, with the recommended addition of Cyclophosphamide (orally at 2 mg / kg per day), which favors the acceleration of the onset of remission and a decrease in the frequency of exacerbations. To avoid infectious complications, Cyclophosphamide is used only in the absence of efficacy from Prednisolone.
In general, treatment is often ineffective. The intensity of the clinical picture can be weakened by the early appointment of Prednisolone in an amount of at least 60 mg / day orally. For pediatric patients, it is appropriate to prescribe normal immunoglobulin for intravenous administration.
The quality of treatment is assessed in the presence of positive dynamics in the clinical course, with the stabilization of laboratory and immunological values and a decrease in the activity of the inflammatory reaction.
Correction or radical elimination of concomitant pathologies that can adversely affect the course of periarteritis nodosa is recommended. Such pathologies include foci of chronic inflammation, diabetes mellitus, uterine fibroids, chronic venous insufficiency, etc.
External treatment for erosions and ulcers involves the use of 1-2% solutions of aniline dyes, epithelizing ointment preparations (Solcoseryl), hormonal ointments, enzyme agents (Iruskol, Himopsin), applicator application of Dimexide. At knots apply dry heat.
Medications
Drugs that are effective in the treatment of periarteritis nodosa:
- Glucocorticoids: Prednisolone 1 mg/kg twice a day orally for 2 months, with a further reduction in dosage to 5-10 mg/day in the morning (day after day) until the disappearance of clinical symptoms. Possible side effects: exacerbation or development of stomach and duodenal ulcers, weakened immunity, edema, osteoporosis, impaired secretion of sex hormones, cataracts, glaucoma.
- Immunosuppressants (if glucocorticoids are ineffective), cytostatics (Azathioprine in the active stage of pathology, 2-4 mg / kg per day for a month, with a further transition to a maintenance dosage of 50-100 mg / day for one and a half to two years), Cyclophosphamide orally 1-2 mg / kg per day for 2 weeks with a further gradual decrease in dosage. With an intensive increase in the pathological process, 4 mg / kg per day are prescribed for three days, then 2 mg / kg per day for a week, with a gradual decrease in dosage over three months. The total duration of therapy is at least one year. Possible side effects: oppression of the hematopoietic system, reduced resistance to infections.
- Pulse therapy in the form of Methylprednisolone 1000 mg or Dexamethasone 2 mg/kg per day intravenously for three days. At the same time, on the first day, Cyclophosphamide is administered at a dosage of 10-15 mg/kg per day.
A combined treatment regimen with the use of glucocorticoids and cytostatics is justified:
- efferent treatment in the form of plasmapheresis, lymphocytopheresis, immunosorption;
- anticoagulant therapy (Heparin 5 thousand units 4 times a day, Enoxiparin 20 mg daily subcutaneously, Nadroparin 0.3 mg daily subcutaneously;
- antiplatelet therapy (Pentoxifylline 200-600 mg per day orally, or 200-300 mg per day intravenously; Dipyridamole 150-200 mg per day; Reopoliglyukin 400 mg intravenously drip, every other day, in the amount of 10 infusions; Clopidogrel 75 mg daily);
- non-steroidal anti-inflammatory drugs, non-selective COX inhibitors (Diclofenac 50-150 mg per day, Ibuprofen 800-1200 mg per day);
- selective COX-2 inhibitors (Meloxicam or Movalis 7.5-15 mg per day daily with meals, Nimesulide or Nimesil 100 mg twice a day, Celecoxib or Celebrex 200 mg per day);
- aminocholine agents (Hydroxychloroquine 0.2 g per day);
- angioprotectors (Pamidin 0.25-0.75 mg three times a day, Xanthinol nicotinate 0.15 g three times a day, for a month);
- enzyme preparations (Wobenzym 5 tablets three times a day for 21 days, then - 3 tablets three times a day for a long time);
- antiviral and antibacterial drugs;
- symptomatic drugs (drugs to normalize blood pressure, to normalize cardiac activity, etc.);
- vasodilators and calcium channel blockers (eg Corinfar).
Therapy with Cyclophosphamide is carried out only if there are strong indications and if glucocorticosteroid agents are ineffective. Possible side effects from taking the drug: myelotoxic and hepatotoxic effects, anemia, sterile hemorrhagic cystitis, severe nausea and vomiting, secondary infection.
Therapy with immunosuppressants should be accompanied by monthly monitoring of blood parameters (general blood count, platelet level, activity of serum liver transaminases, alkaline phosphatase and bilirubin).
Systemic glucocorticosteroids are taken (administered) mainly in the morning, with a mandatory gradual decrease in dosage and an increase in the interval of administration (introduction).
Physiotherapy treatment
Physiotherapy for nodular periarteritis is contraindicated.
Herbal treatment
Despite the fact that periarteritis nodosa is a fairly rare pathology, there are still alternative methods of treating this disorder. However, the possibility of herbal treatment must be agreed in advance with the attending physician, since it is necessary to take into account the severity of the disease and the likelihood of unwanted side effects.
In the early stages of periarteritis nodosa, the use of herbal preparations may be justified.
- Pass through a meat grinder three medium lemons, 5 tbsp. L. Cloves, mixed with 500 ml of honey and pour 0.5 liters of vodka. Everything is mixed well, poured into a jar, closed with a lid and sent to the refrigerator for 14 days. Next, the tincture is filtered and begin to take 1 tbsp. L. Three times a day, half an hour before meals.
- A vegetable equivalent mixture is prepared from tansy, immortelle and elecampane rhizomes. Take 1 tbsp. L. Mixture, pour a glass of boiling water, insist for half an hour. Take 50 ml of infusion three times a day before meals.
- An equivalent mixture is prepared from dried violet flowers, string leaves and dried lingonberries. Pour 2 tbsp. L. Mixture of 0.5 liters of boiling water, insist until cool. Take 50 ml 4 times a day, between meals.
- Mix 1 tbsp. L. Immortelle, wormwood and elecampane, pour 1 liter. Boiling water, insist for two hours. Next, the infusion is filtered and taken three times a day, 100 ml.
A simple and effective way to strengthen the vascular walls with periarteritis nodosa is the regular use of green tea. You should drink 3 cups of the drink every day. Additionally, you can take alcohol tinctures of lure or ginseng, which will help you get rid of unwanted manifestations of the disease as soon as possible. Such tinctures can be bought at any pharmacy.
Surgery
Surgical treatment is not the main one for periarteritis nodosa. The operation can be indicated only in a critical stenosing condition, clinically caused by regional ischemia, or in case of occlusion of the main arterial trunks (Takayasu's arteritis). Other indications for surgical care are:
- thromboangiitis obliterans;
- peripheral gangrene and other irreversible changes in tissues;
- subpharyngeal stenosis in Wegener's granulomatosis (mechanical expansion of the trachea in combination with local use of glucocorticosteroids).
Emergency surgery is prescribed for abdominal complications: intestinal perforations, peritonitis, intestinal infarction, etc.
Prevention
There is no clear concept of the prevention of periarteritis nodosa, since the true causes of the disease are not completely known. You should definitely avoid exposure to factors that can provoke the development of pathology: avoid hypothermia, physical and psycho-emotional overstrain, lead a healthy lifestyle, eat right, protect yourself from bacterial and viral infections.
When the first suspicious signs of the disease appear, you need to visit a doctor as soon as possible: in this case, the chances of diagnosing and treating periarteritis nodosa at the initial stage of its development increase.
Prevention of exacerbations of the disease in patients with remission of periarteritis nodosa is reduced to regular dispensary observation, systematic maintenance and strengthening treatment, elimination of allergens, prevention of self-medication and uncontrolled medication. Patients with vasculitis or periarteritis nodosa should not receive any sera or be vaccinated.
Forecast
In the absence of treatment of nodular periarteritis, death occurs within five years in 95 patients out of a hundred. At the same time, the vast majority of cases of death of patients occur in the first 90 days of the disease. This can happen if the pathology is incorrectly or untimely diagnosed.
The main causes of deaths in periarteritis nodosa are extensive vascular inflammation, the addition of infectious pathologies, heart attack, and stroke.[15]
Timely use of glucocorticoid drugs increases the five-year survival rate by more than half. An even more optimal effect can be achieved by a combination of glucocorticosteroids with cytostatics. If it is possible to achieve the complete disappearance of the symptoms of the disease, then the probability of its exacerbation is estimated at about 56-58%. Damage to the spinal structures and the brain is considered an unfavorable factor for the prognosis.[16]
Genetically determined periarteritis nodosa in childhood is completely cured in about every second case. In 30% of children, the disease has a persistent disappearance of symptoms against the background of constant medical support. Mortality at an early age is 4%: death is due to damage to brain structures, cranial nerves.[17]
Even with a favorable outcome, periarteritis nodosa requires regular rheumatological monitoring. [18]In order to avoid relapses, the patient should beware of infectious diseases, sudden changes in temperature, any self-treatment options. In some cases, relapses can be provoked by pregnancy or abortion.

