
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Churg-Strauss syndrome
Medical expert of the article
Last reviewed: 04.07.2025
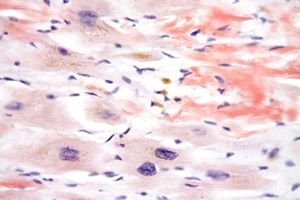
Churg-Strauss syndrome is named after the scientists Churg and Strauss, who first described this disease. The disease is a separate type of vasculitis - allergic angiitis and granulomatosis - affecting mainly medium and small-sized vessels. The disease is also combined with such pathologies as pneumonia, eosinophilia and bronchial asthma. Previously, this pathology was considered an asthmatic type of periarteritis nodularis, but now it is singled out as an independent nosological type.
In 1951, Churg and Strauss (Strauss) first described the syndrome in 13 patients who had asthma, eosinophilia, granulomatous inflammation, necrotizing systemic vasculitis, and necrotizing glomerulonephritis. In 1990, the American College of Rheumatology (ACR) proposed the following six criteria for the diagnosis of Churg-Strauss syndrome:
- Asthma (wheezing, wheezing on exhalation).
- Eosinophilia (more than 10%).
- Sinusitis.
- Pulmonary infiltrates (may be temporary).
- Histologic evidence of vasculitis with extravascular eosinophils.
- Multiple mononeuritis or polyneuropathy.
The presence of four or more criteria has a specificity of 99.7%.
Epidemiology
Approximately 20% of vasculitis from the category of nodular periarteritis are Churg-Strauss syndrome. This pathology begins to develop on average at about 44 years of age. At the same time, men are slightly more likely to get sick with it - 1.3 times.
The incidence of Churg-Strauss syndrome in the United States is 1-3 cases per 100,000 adults per year and about 2.5 cases per 100,000 adults per year worldwide.
Causes of Churg-Strauss syndrome
The causes of this syndrome have not yet been identified. The mechanism of development is based on immune inflammation, destructive and proliferative processes, and in addition to this, on a decrease in the permeability of the vessel walls, the formation of blood clots, the development of ischemia in the area of vascular destruction and hemorrhage. In addition, an important factor in the development of the syndrome is an increased titer of ANCA, which performs antigen neutralization of neutrophil enzymes (mainly proteinase-3, as well as myeloperoxidase). At the same time, ANCA cause a violation of the transendothelial movement of activated granulocytes, and also provoke premature degranulation. Due to changes in the vessels, pulmonary infiltrates appear in organs and tissues with the subsequent development of necrotizing nodular inflammation.
The trigger factors for the development of Churg-Strauss syndrome may be a bacterial or viral infection (for example, nasopharyngeal infection with staphylococci or hepatitis type B), various allergens, intolerance to certain medications, vaccination, excessive cooling, stress, pregnancy or childbirth, as well as insolation.
The presence of HLA-DRB4 may be a genetic risk factor for the development of Churg-Strauss syndrome and may increase the likelihood of developing vasculitic manifestations of the disease.
Risk factors
This disease is quite rare, and although many people fall under risk factors, it develops in only a small percentage of the population. Among such factors are the following:
- Age – most patients with this syndrome are in the 38-52 age group. Only rarely does this pathology develop in elderly people or children;
- The patient has a history of allergic rhinitis or asthma. Most patients with Churg-Strauss syndrome have previously suffered from one of these diseases (and it often occurred in a severe form).
Pathogenesis
The pathogenesis of the disease has not yet been fully studied. But in any case, the fact that it has an allergic and immunopathological nature, often occurs as a result of bronchial asthma, and is also close in symptoms to the nodular form of periarteritis, makes it possible to conclude that the basis for its development are various immunological disorders.
Symptoms of Churg-Strauss syndrome
In addition to the non-specific manifestations that are also observed in the case of nodular periarteritis (this is a state of fever, loss of appetite, weight loss and malaise), the main symptom is a disruption in the functioning of the lungs. As a result, severe bronchial asthma begins, and darkening of the lungs occurs, which is confirmed by chest X-ray, which often quickly disappears - volatile ELI.
Among the main symptoms of the pathology is the GRB syndrome, which is usually a precursor to the appearance of clinical signs of systemic vasculitis. Also often observed is the addition of infectious lung pathologies with the subsequent development of bronchial asthma of the infection-dependent type, as well as bronchiectatic disease. Pulmonary infiltrates are observed in 2/3 of patients with the syndrome. About a third of patients are diagnosed with pleurisy with an increase in the number of eosinophils in the pleural fluid.
When the gastrointestinal tract is affected, abdominal pain, diarrhea, and, in rare cases, bleeding begin to appear. The development of these symptoms is provoked by either eosinophilic gastroenteritis or vasculitis of the intestinal wall. The latter disease can cause peritonitis, complete destruction of the intestinal wall, or intestinal obstruction.
Clinical manifestations of cardiac disorders occur in 1/3 of all patients, but they are detected at autopsy in 62% of cases, and this is the cause of death in 23% of cases. Various changes in ECG readings are observed in about half of patients. About 1/3 of all cases of the disease are accompanied by the development of heart failure or pericarditis in acute or constrictive form. Rarely, patients experience increased blood pressure and myocardial infarction.
Skin diseases are observed in 70% of patients - with SCS this is a more common symptom than with nodular periarteritis. Among the manifestations:
- Hemorrhagic rash;
- Nodes on and under the skin;
- Redness of the skin;
- Hives;
- Microabscesses of the skin;
- Livedo reticularis.
Kidney disease is the least common symptom. However, it is not as dangerous as in the case of Wegener's granulomatosis or periarteritis nodosa. About half of patients with the syndrome suffer from focal nephritis, which often causes arterial hypertension. Patients with antineutrophil antibodies in the plasma may develop necrotizing glomerulonephritis.
Joint diseases (such as polyarthralgia or polyarthritis) occur in half of all patients with this syndrome. They usually develop non-progressive migratory arthritis, which affects both small and large joints. In some cases, myositis or myalgia is observed.
Stages
Churg-Strauss syndrome usually goes through 3 main stages (conditionally) as it develops.
In the initial period (it can last for 30 years), patients suffer from frequent allergies, including asthma, hay fever, and rhinitis.
In stage 2, the number of eosinophils in tissues and blood begins to increase. At this stage, patients are often diagnosed with Loeffler syndrome, pulmonary infiltration with eosinophilia, or eosinophilic gastroenteritis.
At the third stage, patients exhibit clinical manifestations of systemic vasculitis.
Complications and consequences
Among the complications of the disease, the most dangerous is pneumonia, which develops under the influence of Pneumocystis carini.
SCS is dangerous because it affects various organs, including the heart, lungs, skin, gastrointestinal tract, muscles, joints, and kidneys. If left untreated, this disease can lead to death. Possible complications of the disease:
- Disruption of peripheral nerve function;
- Itching and ulceration of the skin, as well as infectious complications;
- Inflammation of the pericardium, development of myocarditis, and in addition, heart failure and heart attacks;
- Glomerulonephritis, in which the kidneys gradually lose their filtration function, resulting in renal failure.
Risk stratification
The French Vasculitis Study Group has developed a five-point (five-factor) system that predicts the risk of death in Churg-Strauss syndrome using clinical features. These factors are:
- Decreased renal function (creatinine> 1.58 mg/dL or 140 μmol/L)
- Proteinuria (> 1 g/24 hours)
- Gastrointestinal bleeding, heart attack, or pancreatitis
- Central nervous system damage
- Cardiomyopathy
The absence of any one of these factors indicates a milder course, with a five-year mortality rate of 11.9%. The presence of one factor indicates severe disease, with a five-year mortality rate of 26%, and two or more indicate very severe disease: 46% mortality at five years.
Diagnostics of Churg-Strauss syndrome
Among the main diagnostic criteria are symptoms such as eosinophilia, bronchial asthma, and a history of allergies. In addition, eosinophilic pneumonia, neuropathy, inflammation of the paranasal sinuses, extravascular eosinophilia. If the patient has at least 4 of these diseases, SCS can be diagnosed.
 [ 31 ], [ 32 ], [ 33 ], [ 34 ]
[ 31 ], [ 32 ], [ 33 ], [ 34 ]
Tests
Blood is taken for a general analysis: to diagnose the disease, there should be an excess of eosinophils by 10% above the norm, as well as an acceleration of the erythrocyte sedimentation process.
A general urine test should reveal the presence of protein in the urine, as well as an increase in the number of red blood cells.
Transbronchial, skin and subcutaneous tissue biopsy: in this case, pronounced eosinophil infiltration in the walls of small vessels should be detected, as well as necrotizing granulomatous processes in the respiratory organs.
Immunological analysis to detect increased levels of ANCA antibodies. The focus here is on increasing levels of total IgE as well as perinuclear antibodies with antimyeloperoxidase activity.
Instrumental diagnostics
CT scan of the lungs – the process involves visualization of parenchymatous clusters, mainly located on the periphery; it is also noticeable that the walls of the bronchi have thickened, with expansion in some places, bronchiectasis is noticeable.
Microscopy of exudate in the pleural fluid, as well as therapeutic bronchoscopy to detect eosinophilia.
Conducting an echocardiogram to detect symptoms of mitral regurgitation, as well as the proliferation of connective tissue with the appearance of scars in the heart muscle.
Who to contact?
Treatment of Churg-Strauss syndrome
Treatment of SCS is complex - cytostatics and glucocorticosteroids are used in the course of therapy. In general, the treatment is similar to the principles of therapy of nodular periarteritis.
Drug treatment
In case of damage to the gastrointestinal tract, as well as lungs, kidneys and skin, treatment should be started with prednisolone. The therapeutic dose is 60 mg/day. After 1-2 weeks of such administration, a transition to periodic use of prednisolone with a gradual reduction in the dose occurs. After 3 months, if an improvement in the condition was noted, the dosage continues to be reduced, bringing it to a maintenance dose, which is left for a long period.
If prednisolone has had no effect, and also in the event of symptoms of diffuse CNS disorder, blood flow insufficiency and conduction disorders, hydroxyurea is prescribed internally at a dosage of 0.5-1 g/day. If the number of leukocytes has decreased to 6-10x109/l, it is necessary to switch to using the drug in a regimen every 2 days, on the third day or stop taking it for 2-3 months. Other cytostatics can also be used - such as cyclophosphamide or azathioprine.
If the patient has bronchial asthma, bronchodilators are prescribed.
Anticoagulants or antiplatelet agents (such as acetylsalicylic acid at a dosage of 0.15-0.25 g/day or curantil at a dosage of 225-400 mg/day) are used as a preventive measure against the development of thromboembolic complications.
A systematic review conducted in 2007 showed the effectiveness of high-dose steroids.
Vitamins
Since corticosteroids negatively affect bone strength, it is necessary to replace the loss by taking the required amount of calcium, as well as consuming approximately 2000 IU of vitamin D per day.
Forecast
Churg-Strauss syndrome without timely treatment has an unfavorable prognosis. In case of multiple organ damage, the disease progresses very quickly, increasing the risk of death as a result of heart and lung dysfunction. Adequate treatment allows for 5-year survival in 60-80% of patients.
The main causes of death in Churg-Strauss syndrome are myocarditis and myocardial infarction.

