Medical expert of the article
New publications
Biopsy of the lymph node
Last reviewed: 05.05.2022

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
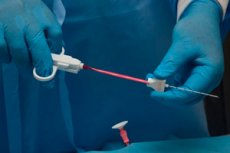
In order to understand the causes of enlarged lymph nodes, it is necessary to conduct a series of diagnostic studies. The most informative and common diagnostic method is currently considered a biopsy of the lymph node. This is a procedure during which a piece of biomaterial is removed for further research.
In the human body, the lymph nodes play the role of a kind of filtering stations that attract and neutralize pathogens. When pathogens enter the node, it increases, which is also characteristic of inflammatory reactions or malignant processes. To understand what kind of pathology occurs in the lymphatic link, and perform a procedure such as a biopsy. [1]
What is the difference between a puncture and a biopsy of the lymph nodes?
Histological analysis is prescribed for the diagnosis of many pathologies, since it successfully helps to determine the type of the disease process, identify its phase, differentiate the tumor, etc. Often, it is this study that makes it possible to accurately establish the diagnosis and prescribe the correct treatment.
Lymph nodes are the main links of the body's immune system. These are "warehouses" of specific tissue that ensures the maturation of T and B-lymphocytes, forms plasma cells that produce antibodies, and also cleanses the lymph. Bacteria and foreign particles are filtered through the lymph flow in the lymph nodes. With their excess, the body's defense mechanism is activated, immunoglobulins are produced, and cellular memory is formed. All these reactions are an integral part of immunity, the elimination of infectious and malignant agents.
Such protection normally always works, and the person himself may not be aware that such reactions occur in his body. Only with a massive attack or with a drop in immunity, the nodes can increase, pain may appear. However, in most patients, everything returns to normal after a few days.
If several groups of lymph nodes increase at once, the patient's state of health deteriorates sharply, the temperature rises, other painful signs appear, then in such a situation a diagnosis is required, including a biopsy or puncture of the lymph node. Often these concepts are taken as synonyms, but this is not entirely true.
If they talk about a puncture puncture, which involves the collection of a liquid secret with cells for further cytological examination, then the term "puncture" is usually used. A biopsy is mentioned if it involves the removal of a large portion of the biomaterial with subsequent histological analysis.
Puncture is a minimally invasive, fine-needle procedure that is virtually painless. A lymph node biopsy requires a more traumatic intervention, often with a scalpel. However, there is also the concept of "puncture biopsy", in which the node is pierced with a thicker needle device, which allows to select the required amount of tissue.
Indications for the procedure
When diagnosing lymphoproliferative and malignant pathologies, it is important not only to confirm the diagnosis morphologically, but also to detail it by cytology and histology. Similar information can be obtained with the help of puncture and biopsy of the lymph node.
The puncture is used as an approximate diagnostic manipulation. Puncture is not suitable for determining lymphoproliferative pathology: a biopsy (either excisional or puncture) is required, with further cytological and histological examination of the biopsy.
Indications for puncture may be:
- an enlarged single lymph node, without formed conglomerates and without signs of lymphoproliferative pathology;
- Ultrasound signs of liquid formation;
- the need to remove biomaterial for an auxiliary examination after performing a biopsy.
A lymph node biopsy is a surgical procedure that is performed using local or general anesthesia. As a result of the procedure, a particle of the lymphatic link, or the entire node, is obtained for further research. Microscopic analysis is the key to accurate and correct diagnosis.
The main indications for a biopsy are:
- high risks of developing a tumor process according to clinical information;
- lymphadenopathy of unknown origin (all the diagnostic methods involved did not help in making a diagnosis);
- lack of effectiveness of the therapy.
It is impossible to say exactly at what size of the lymph node a biopsy is mandatory. However, most experts believe that a lymph node larger than 30 mm, and this is not associated with an infectious process, requires a biopsy.
Sometimes one biopsy study is not enough: the patient is prescribed repeated procedures. This is possible if multiple histological changes were found during the previous biopsy:
- necrosis of the lymph node;
- sinus histiocytosis;
- sclerosis;
- paracortical response with the presence of a large number of macrophages and plasma cells.
Preparation
The preparatory stage before a lymph node biopsy may include consulting a general practitioner, surgeon, endocrinologist, anesthetist, oncologist, and hematologist. It is mandatory to perform a general and biochemical blood test, a study of the blood coagulation system.
An ultrasound examination is prescribed to clarify the location of the pathological focus.
The doctor conducts a conversation with the patient in advance:
- clarifies the allergic status;
- receives information about the medications taken;
- in women, it clarifies the phase of the menstrual cycle and excludes the possibility of pregnancy.
If the patient takes drugs that thin the blood, then they are canceled 7-10 days before the biopsy.
If the procedure will be performed using general anesthesia, then the preparation is carried out more carefully:
- it is forbidden to eat and drink on the day of the intervention;
- dinner on the eve should be as light as possible, with the use of mainly plant-based easily digestible food;
- 2-3 days before the intervention, you should not take alcohol, it is undesirable to smoke;
- the next morning, before going to the biopsy procedure, the patient should take a shower without the use of lotions and body creams.
Technique of the lymph node biopsy
A biopsy of shallow lymph nodes is usually short in time - for many patients, the procedure is completed in about 20 minutes. Local anesthesia is usually used, although the puncture is generally considered painless. If ultrasound control is used, then the doctor, using an ultrasonic sensor, specifies the location of the painful structure, puts a special mark, which is reflected on the monitor. The skin in the puncture zone is treated with an antiseptic, and then with an anesthetic, or an anesthetic is injected. The patient lies on the couch horizontally, or is in a sitting position. If a biopsy is performed in the neck, then it is fixed in a special way, and the patient is explained about the need to temporarily not perform swallowing movements. The patient must remain completely still during the biopsy.
After taking the required amount of biological material, the puncture zone is treated with an antiseptic. It may be recommended to apply a cold dry compress for half an hour.
There is no need for a long stay in the clinic, or placing the patient in a hospital: he can go home on his own if there are no other reasons for keeping him. For the first time after the procedure, it is important to avoid physical activity.
If a deep site biopsy is required, general anesthesia may be required. In such a situation, the patient after the diagnosis is not sent home, but remains in the clinic - from several hours to 1-2 days.
An open biopsy requires a special set of tools: in addition to a scalpel, these are clamps, a coagulating apparatus, and materials for suturing. This intervention lasts up to 60 minutes. The doctor selects the lymph node necessary for the biopsy, fixes it with his fingers, then performs a 4-6 cm incision in the skin. It dissects the subcutaneous fat layer, pushes the muscle fibers, the network of nerves and blood vessels. If it is required to remove one or more nodes during a biopsy, the surgeon preliminarily bandages the vessels to prevent bleeding, lymph leakage, and the spread of tumor cells (if we are talking about a malignant process). After removing the lymph nodes, the doctor sends them for examination, once again conducts an audit of the wound, and sutures the incisions. In some cases, a draining device is left, which is removed after 24-48 hours. Removal of sutures is carried out within a week. [2]
How is a lymph node biopsy performed?
Taking a biopsy in a particular lymph node may have its own characteristics, which depends on the location, the depth of the structure, as well as the presence of vital organs and large vessels near the damaged link.
- A biopsy of the lymph node in the neck can be prescribed for otolaryngological, dental problems - the most common causes of lymphadenopathy. If lymphadenopathy has an unclear origin, then ultrasound is prescribed first, and only after that, if necessary, a biopsy. Lymph nodes increase in malignant tumors, as cancer cells penetrate into the lymphatic vessels that drain a separate area. In the future, these cells settle in the filter nodes, like metastases, and begin to develop. Often in oncology, the defeat of the lymph nodes occurs "along the chain", which is perfectly determined by probing. A biopsy on the neck can be performed either with a needle puncture with the removal of material, or with an operative access with complete removal of the link for histological analysis.
- A sentinel lymph node biopsy for melanoma is performed similarly to a biopsy for breast cancer. If there is information about metastasis to distant organs and lymph nodes, then performing a biopsy is considered useless. In the absence of metastases, a sentinel node biopsy is warranted. It is usually done after the removal of the melanoma itself. It is possible to visualize the lymph node using various radiological methods.
- A biopsy of the axillary lymph node is performed with the patient in a sitting position, who raises his arm up and takes it back a little. Most often, this procedure is carried out with a lesion of the mammary gland: lymph flows through the vessels to the nodes located in the armpit on the same side. Such lymph nodes form a kind of axillary-nodal chain. Its defeat plays an important role in planning a treatment regimen for breast pathology. The study is also appropriate for melanoma or squamous cell carcinoma of the upper limb, with Hodgkin's disease. [3]
- A biopsy of the inguinal lymph nodes is performed from the position of the patient lying on the couch, the leg (right or left, depending on the side of the lesion) is retracted to the side. Such a study is most often prescribed for suspected tumor processes (cancer of the testicles, vulva, cervix, prostate, bladder, rectum), or if it is not possible to find out the cause of lymphadenopathy in other ways (for example, with lymphogranulomatosis or HIV- infections).
- A biopsy of the supraclavicular lymph node is always caused by suspicions of quite serious pathologies: in many cases, these are tumors - metastases of cancer or lymphoma located in the chest or abdominal cavity. The supraclavicular lymph node on the right side can make itself felt in tumor processes of the mediastinum, esophagus, lung. Lymph from the intrathoracic organs and the abdominal cavity approaches the lymph node on the left side. Inflammatory diseases can also cause supraclavicular lymphadenopathy, but this happens much less frequently.
- A biopsy of the mediastinal lymph node is performed in the projection area of the upper third of the intrathoracic tracheal region, from the upper edge of the subclavian artery or pulmonary apex to the point of intersection of the upper border of the left brachiocephalic vein and the middle tracheal line. The most common indications for mediastinal lymph node biopsy are lymphoproliferative neoplasms, tuberculosis, and sarcoidosis.
- A biopsy of a lymph node in the lung is a common procedure for cancer, tuberculosis, and sarcoidosis. Often, lymphadenopathy becomes the only sign of pathology, since many pulmonary diseases are asymptomatic. In any case, before establishing a definitive diagnosis, the doctor must perform a biopsy and obtain histological information.
- A biopsy of the abdominal lymph nodes is prescribed for suspected tumor processes in the gastrointestinal tract, organs of the female and male reproductive organs, and the urinary system. Often, enlarged abdominal lymph nodes are noted with hepatosplenomegaly. A biopsy is done for both primary and differential diagnosis. A large number of lymph nodes in the abdominal cavity are located parietal along the peritoneum, along the vessels, in the mesentery and along the intestine, near the omentum. Their increase is possible with damage to the stomach, liver, intestines, pancreas, uterus, appendages, prostate, bladder.
- A biopsy of the submandibular lymph node can be prescribed for pathologies of the teeth, gums, cheeks, laryngeal region and pharynx, if the cause of the lymphadenopathy cannot be found, as well as if metastases of the cancerous process or lymphoma are suspected.
- A biopsy for cancer of the lymph nodes is performed in the absence of metastases to distant organs and lymph nodes. Otherwise, the procedure is considered meaningless for the patient. If there is no distant metastasis, then they proceed, first of all, to the study of the first in the chain, the "sentinel" lymph node.
- A biopsy of the retroperitoneal lymph node is appropriate for malignant processes in the male and female genital area. Approximately 30% of patients already at the first stage of cancer have microscopic metastases in the lymph nodes that cannot be identified using computed tomography or markers. A biopsy is performed, as a rule, from the side where the primary tumor focus was located. The procedure is usually performed as part of a retroperitoneal lymphadenectomy.
- A biopsy of the intrathoracic lymph nodes is a mandatory study for suspected cancer of the lungs, esophagus, thymus, breast, lymphoma and lymphogranulomatosis. In the nodes of the mediastinum, metastases from the abdominal cavity, pelvis, retroperitoneal space (kidneys, adrenal glands) in advanced stages can also spread.
- Biopsy of the paratracheal lymph nodes is often performed in patients with lung cancer. Paratracheal lymph nodes are located between the upper mediastinal and tracheobronchial nodes. In the primary tumor process on the same side, they are divided as ipsilateral, and in the absence of a primary tumor, as contralateral.
Lymphatic fluid flows through the corresponding vessels. If cancer cells get into it, then they are, first of all, in the first lymph node of the chain. This first node is called the sentinel or signal node. If cancer cells are not found in the sentinel lymph node, then subsequent nodes should in theory be healthy.
Types of biopsies
There are several types of biopsy of the lymph nodes, which depends on the technique for removing the biomaterial. Some types of procedures are performed in stages: first, a needle puncture is performed, and then an open intervention, if the puncture was not enough for diagnosis. An open biopsy method is required if the result of cytology turned out to be uncertain, doubtful, approximate.
- Open biopsy of the lymph node is the most complex and invasive option for such a diagnosis. During the procedure, a scalpel is used, and the entire node is selected for research, and not just part of it. Such an intervention is often the only correct one if malignant processes are suspected.
- Puncture biopsy of the lymph node is a relatively gentle and painless procedure that does not cause much discomfort to patients. During the diagnostics, a mandrin is used, which plays the role of a stylet. With the help of a mandrin, the required amount of biomaterial is cut off and captured. Needle biopsy involves the use of local anesthesia, does not require the patient to be placed in a hospital.
- Excisional lymph node biopsy is a term often applied to an open biopsy performed under general anesthesia. The affected node is removed through an incision.
- Trepan biopsy of the lymph node involves the use of a special large needle with notches that allow you to remove a particle of tissue of the required size.
- A fine-needle biopsy of a lymph node is called an aspiration biopsy: it involves the use of a thin hollow needle device. Usually, the node is probed and pierced: if this is not possible, then ultrasonic control is used. As a rule, a fine-needle biopsy is prescribed if it is necessary to study the submandibular or supraclavicular lymph nodes, if metastases of lymphoid structures are detected.
Biopsy of lymph nodes under ultrasound control
Currently, experts consider the targeted puncture procedure, or the so-called “ultrasound-guided biopsy”, to be the most acceptable technique for lymph node biopsy.
We are talking about the process of removing a biomaterial sample, which is performed under ultrasound supervision: as a result, the location and insertion of the puncture needle is carried out more accurately and safely. This is extremely important for the doctor, since often a suspicious lymph node is located in deep tissues near vital organs, or is small, which greatly complicates the procedure.
Ultrasound observation helps to insert the instrument precisely into the required place, without the risk of damage to adjacent tissues and organs. As a result, the risk of complications is minimized.
In what way the required zone is visualized, the doctor determines. An additional advantage of the technique is not only safety, but also its cheapness: no ultra-modern and expensive equipment is needed.
A biopsy with ultrasound is especially recommended if it is necessary to examine not only the affected structure, but also to find out the peculiarities of the blood circulation near it. This approach will avoid injury to blood vessels, exclude the release of blood into the tissue.
For the procedure, special needles with end sensors are used. This simple device helps to clearly monitor the position of the needle and its progress.
The recovery period after such an intervention is faster and more comfortable for the patient. [4]
Contraindications to the procedure
Before referring the patient for a biopsy of the lymph node, the doctor will prescribe a number of studies and tests that are necessary to exclude contraindications to this procedure. The basic preliminary diagnosis is a general blood test and an assessment of the quality of coagulation. A biopsy is not performed with a tendency to bleeding - for example, in patients suffering from hemophilia, since vessels may be injured during the intervention.
Biopsy of the lymph node is contraindicated in case of purulent processes in the puncture area. It is undesirable to do the procedure for pregnant or lactating women, as well as during menstrual bleeding.
In general, experts distinguish the following list of contraindications:
- disorders of the blood coagulation system (congenital disorders, acquired or temporary - that is, associated with the intake of appropriate blood thinning medications);
- platelet count below 60 thousand per µl;
- hemoglobin level is less than 90 g/liter;
- INR greater than 1.5;
- prothrombin time exceeding the norm by 5 seconds;
- infectious and inflammatory processes in the area of the biopsy;
- monthly bleeding in women on the day of the procedure;
- decompensated chronic pathologies;
- treatment with non-steroidal anti-inflammatory drugs during the last week.
Normal performance
Microscopic examination of a patient's lymph node biopsy is considered the most important in the diagnostic aspect of oncological pathologies, it helps to assess the quality of drug therapy.
Histology of the lymph nodes is a minor surgical intervention, during which a small piece of tissue is taken away for further examination. With the help of a biopsy of the lymph node, specialists can study the features of its structure, detect painful abnormalities, and notice signs of an inflammatory reaction.
The lymph node is the basic link of the defense system in the body, which is the connecting element between the lymphatic vessels. Lymph nodes allow you to overcome the infectious invasion by producing leukocytes - specific blood cells. In the node, a microbial and viral infection, malignant cells are captured.
A biopsy of the lymph node helps to identify the presence of atypical cells, to determine the specifics of the infectious inflammatory process, benign tumors, and purulent pathologies. The biopsy is most often performed in the inguinal, axillary, mandibular, and behind the ear regions.
A biopsy is prescribed for patients who need to find out the type of tumor process - especially if a malignant pathology is suspected. Often, diagnostics are prescribed to determine infectious diseases.
The results of a biopsy of the lymph node
After examining the biopsy (material obtained by biopsy of the lymph node) and detecting particles of pathology, specialists begin to count cell structures and display a lymphadenogram. For this purpose, the immersion method of microscopic observation is used, which makes it possible to differentiate at least half a thousand cells and calculate their percentage presence.
These lymphadenograms are extremely necessary and valuable for the diagnosis of a nonspecific form of lymphadenitis.
Norm of lymphadenogram results:
|
Content of relevant cell types |
Percentage |
|
Lymphoblasts |
0.1 to 0.9 |
|
Prolymphocytes |
5.3 to 16.4 |
|
Lymphocytes |
67.8 to 90 |
|
Reticular cells |
0 to 2.6 |
|
Plasma cells |
0 to 5.3 |
|
Monocytes |
0.2 to 5.8 |
|
Mast cell |
0 to 0.5 |
|
Neutrophil granulocytes |
0 to 0.5 |
|
Eosinophilic granulocytes |
0 to 0.3 |
|
Basophilic granulocytes |
0 to 0.2 |
In the biological material removed during the biopsy of the lymph node, there are predominantly mature lymphocytes with prolymphocytes. Their total number can be from 95 to 98% of all cellular structures.
Reactive lymphadenitis is manifested by an increase in the number of reticular cells, the detection of macrophages and immunoblasts.
In acute lymphadenitis, an increase in the number of macrophages and neutrophils is observed.
Complications after the procedure
Usually, a diagnostic lymph node biopsy passes without any difficulties. Only in some cases complications develop:
- bleeding due to accidental vascular injury during biopsy;
- secretion of lymph from the wound;
- paresthesia, violation of the sensitivity of the area of intervention;
- infection associated with the ingress of an infectious agent - in particular, during the procedure;
- trophic disorders associated with mechanical injuries of the nervous structures.
Some patients may have impaired consciousness, dizziness, weakness. The condition should return to normal within 1-2 days.
Dangerous symptoms requiring urgent medical attention:
- fever, fever;
- the appearance of a strong, throbbing, growing pain in the area of the biopsy of the lymph node;
- discharge of blood or pus from the wound;
- redness, swelling of the biopsy site.
Consequences after the procedure
A lymph node biopsy is not performed if the patient has any contraindications. Otherwise, adverse effects may develop. For example, if a person suffers from disorders of the blood coagulation system, even a simple needle biopsy can result in bleeding.
In order to prevent the occurrence of post-procedural problems, a lymph node biopsy should be performed by a specialist, in compliance with all the required conditions, aseptic and antiseptic rules.
In some cases, the following troubles may occur:
- joining the infection;
- bleeding of the wound;
- nerve damage.
However, the percentage of development of negative consequences is relatively small. But the information obtained during the biopsy is of great value to the doctor, allowing you to make the correct diagnosis and prescribe the appropriate effective treatment.
Care after the procedure
Usually, the lymph node biopsy procedure is not difficult and is well tolerated by patients. After removal of the biomaterial by aspiration or puncture, only the puncture site remains on the skin, which is treated with an antiseptic solution and sealed with a plaster. If an open biopsy was performed, then the wound is sutured and bandaged. Removal of sutures is carried out throughout the week.
The wound after a biopsy of the lymph node should not be wetted. It is necessary to treat with antiseptic solutions to prevent infection. If the body temperature suddenly rises, the intervention site swells, bleeds, or bothers in any other way, then you need to urgently visit a doctor.
The appearance of short, mild pain after the procedure is allowed.
What not to do after a biopsy of the lymph nodes:
- to take a bath;
- swim in pools, open water;
- visit a bath or sauna;
- practice vigorous exercise.
These restrictions apply for approximately 2 weeks after the procedure, depending on the type and extent of the intervention, such as a lymph node biopsy.

