
All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Abdominal abscess
Medical expert of the article
Last reviewed: 04.07.2025
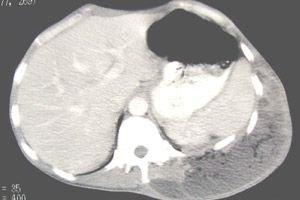
An abdominal abscess is an inflammation of the abdominal organs of a purulent nature with their subsequent melting and the formation of a purulent cavity of varying size with the presence of a pyogenic capsule. It can form in any part of the abdominal cavity with the formation of a number of clinical syndromes: septic, intoxication, febrile.
Epidemiology
The number of surgical interventions performed on abdominal organs is constantly growing. This, the use of a huge number of various antibiotics, as well as a strong weakening of the body's immune system due to rapid urbanization leads to the frequent development of postoperative abdominal abscesses. According to statistics, postoperative complications in the form of abscess formation develop in 0.8% of patients after planned abdominal surgeries and in 1.5% after emergency operations.
Causes abdominal abscess
As a rule, abdominal abscesses develop after various injuries, infectious diseases of the gastrointestinal tract, inflammatory processes in the organs located in the abdominal cavity, as well as as a result of perforation of a defect in a stomach ulcer or duodenal ulcer.
Main reasons:
- Consequence of secondary peritonitis (perforated appendicitis; anastomotic failure after abdominal surgery, pancreatic necrosis after surgery, traumatic injuries), etc.
- Inflammation of the internal female genital organs of a purulent nature (salpingitis, inflammation of the ovarian appendages, purulent parametritis, pyosalpinx, tubo-ovarian abscesses).
- Acute pancreatitis and cholecystitis, nonspecific ulcerative colitis.
Osteomyelitis of the spine, spondylitis of tuberculous etiology, inflammation of the perirenal tissue.
The main pathogens of abscesses are aerobic (Escherichia coli, Proteus, Staphylococcus and Streptococcus, etc.) and anaerobic (Clostridium, Bacteroides fragilis, Fusobacteriales) bacterial flora.
Risk factors
Very often, abdominal abscesses develop as a result of surgical interventions on abdominal organs (most often, after operations on the bile ducts, pancreas, intestines). There are cases when the peritoneum becomes infected after the intervention, especially in case of anastomosis failure.
In 70% of cases, an abscess develops in the intraperitoneal or retroperitoneal region; in 30%, it is localized inside an organ.
 [ 11 ], [ 12 ], [ 13 ], [ 14 ], [ 15 ], [ 16 ], [ 17 ], [ 18 ]
[ 11 ], [ 12 ], [ 13 ], [ 14 ], [ 15 ], [ 16 ], [ 17 ], [ 18 ]
Pathogenesis
An abdominal abscess develops as a result of the hyperreactivity of the immune system with active growth and reproduction of streptococcal and staphylococcal flora, as well as E. coli (appendicular abscess). Pathogens penetrate the abdominal cavity by the lymphogenous or hematogenous route, as well as by contact through the fallopian tubes, when there is destructive inflammation of the organs or organ, injury, perforation, failure of the sutures that were applied during surgical intervention.
The main difference of an abdominal abscess is the fact that the inflammation focus is clearly delimited from the healthy tissues that surround it. If the pyogenic membrane is destroyed, sepsis and purulent leaks develop. Abscesses can be either single or multiple.
Symptoms abdominal abscess
The first signs of an abdominal abscess vary, but in most cases, patients experience:
- A sharp fever, chills, which are accompanied by mild pulling sensations in the abdominal area, which intensify upon palpation.
- Frequent urge to urinate (since the abdominal cavity is located close to the bladder.
- Constipation.
- Nausea, which may be accompanied by vomiting.
Also, other objective symptoms of an abdominal abscess are:
- Tachycardia, high blood pressure.
- Tension of the muscles of the anterior abdominal wall.
If the abscess is subdiaphragmatic, then the main symptoms also include:
- Pain in the hypochondrium area, which may intensify during inhalation and radiate to the shoulder blade.
- By changing the patient's gait, he begins to tilt his body towards the side of discomfort.
- High body temperature.
Complications and consequences
If an abdominal abscess is not diagnosed in time and proper treatment is not started, quite serious consequences may arise:
- Sepsis.
- Peritonitis.
- Breakthrough of pus into the pleural cavity or peritoneum.
That is why, if you feel any discomfort or pain in the abdominal area, you should immediately seek help from a gastroenterologist or therapist.
Diagnostics abdominal abscess
The main diagnostic methods are:
- X-ray of the chest and abdominal organs.
- Ultrasound examination.
- CT and MRI as auxiliary diagnostic methods.
- Taking a puncture from the posterior vaginal fornix or the anterior wall of the rectum (if there is a suspicion of the development of an abscess of the Douglas zone).
 [ 34 ], [ 35 ], [ 36 ], [ 37 ], [ 38 ], [ 39 ]
[ 34 ], [ 35 ], [ 36 ], [ 37 ], [ 38 ], [ 39 ]
Tests
If an abscess cannot be diagnosed due to the absence of any symptoms, tests may be prescribed, including a complete blood count. With this disease, the patient almost always has leukocytosis, sometimes neutrophilia (a sharp shift in the leukocyte formula to the left), as well as an increase in ESR.
 [ 40 ], [ 41 ], [ 42 ], [ 43 ], [ 44 ], [ 45 ], [ 46 ]
[ 40 ], [ 41 ], [ 42 ], [ 43 ], [ 44 ], [ 45 ], [ 46 ]
Instrumental diagnostics
Chest X-rays may show that the diaphragm dome is elevated on the affected side. Reactive effusion may be seen in the pleural area. In subdiaphragmatic abscesses, a gas bubble and fluid level below it may be seen on X-rays.
Ultrasound signs of abdominal abscess
The "gold" standard for diagnosing abdominal abscesses of various localizations is ultrasound examination. Ultrasound signs are: a clearly defined liquid formation in the capsule, the contents of which are heterogeneous and look like a threadlike structure or echogenic suspension. The so-called gas reverberation effect occurs, when multiple reflections of sound gradually reduce its intensity.
Treatment abdominal abscess
Treatment involves surgery to remove the abscess and drain it using a catheter.
Medication does not cure an abdominal abscess, but various antibiotics can limit the spread of infection. That is why doctors prescribe them to patients before and after surgery. They mainly use drugs that can suppress the development of intestinal microflora. In some cases, antibiotics that are active against anaerobic bacteria, including Pseudormonas, are also recommended.
Medicines
Metronidazole. An effective antimicrobial and antiprotozoal agent. The drug contains the active substance metronidazole. It is capable of reducing the 5-nitro group of intracellular proteins in protozoa and anaerobic bacteria. After reduction, this nitro group interacts with the DNA of bacteria, as a result of which the synthesis of nucleic acids of pathogens is inhibited and they die.
Metronidazole is effective against amoebae, trichomonas, bacteroides, peptococci, fusobacteria, eubacteria, peptostreptococci and clostridia.
Metronidazole has a high absorption and effectively penetrates into the affected tissues and organs. The dosage is individual and is determined by the attending physician depending on the patient's condition. Patients with metronidazole intolerance, a history of epilepsy, diseases of the central and peripheral nervous system, leukopenia, and abnormal liver function are prohibited from using the drug. It should also not be prescribed during pregnancy.
In some cases, the use of the drug may cause: vomiting, anorexia, diarrhea, glossitis, pancreatitis, migraines, vertigo, depression, allergies, dysuria, polyuria, candidiasis, frequent urination, leukopenia.
Prevention
Preventive measures are based on adequate and timely treatment of various diseases of organs located in the abdominal cavity. It is also very important to make a correct diagnosis in acute appendicitis in time and perform an operation to remove it.
 [ 47 ], [ 48 ], [ 49 ], [ 50 ], [ 51 ], [ 52 ], [ 53 ], [ 54 ], [ 55 ], [ 56 ]
[ 47 ], [ 48 ], [ 49 ], [ 50 ], [ 51 ], [ 52 ], [ 53 ], [ 54 ], [ 55 ], [ 56 ]

